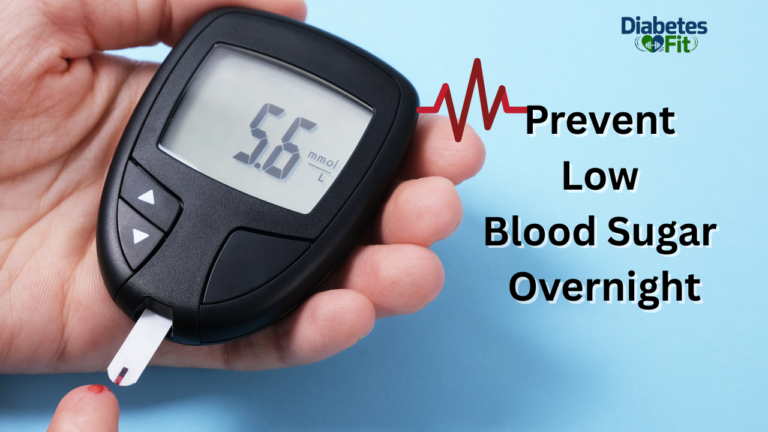
Does Hypoglycemia Cause Weight Gain? The Surprising Truth
I’ll be straight with you: if you’ve been dealing with low blood sugar episodes and watching the number on the scale climb, you’re not imagining things. But the connection between hypoglycemia and weight gain isn’t what most people think.
Hypoglycemia doesn’t directly cause weight gain. Your body doesn’t magically create extra pounds when your blood sugar drops. What happens instead is more subtle—and honestly, more frustrating. The way you respond to low blood sugar, combined with the survival mechanisms your body kicks into gear, can absolutely lead to gaining weight over time.
Understanding whether hypoglycemia can cause weight gain is crucial for managing your health effectively. Many people wonder, does Hypoglycemia Cause Weight Gain?
Let me explain how this actually works in real life.
What Really Happens When Your Blood Sugar Crashes
Picture this: it’s 11 a.m., you skipped breakfast, and suddenly you’re sweating, shaking, and would literally fight someone for a candy bar. That’s hypoglycemia in action.
When your blood glucose drops below normal (usually under 70 mg/dL), your body freaks out a little. Your brain needs glucose to function, so this is essentially an emergency situation. Your system floods with stress hormones—adrenaline and cortisol—designed to quickly raise your blood sugar back up.
These hormones don’t just tap politely on your shoulder. They scream at you to eat something, and fast. You’re not craving a sensible chicken salad. You want sugar, bread, something that hits your bloodstream immediately. This is pure biology, not a lack of willpower.
The Vicious Cycle That Leads to Extra Pounds
Here’s where the weight gain sneaks in. When you’re in the middle of a hypoglycemic episode, rational portion control goes out the window. You feel terrible—dizzy, anxious, maybe even nauseous—and you just want it to stop.
So you eat. And you probably eat more than the 15 grams of carbs technically needed to correct low blood sugar. Maybe you grab a bagel, a muffin, and a juice box. Who could blame you? But that’s potentially 300-400 calories in a single sitting, driven entirely by your body’s panic response.
Then comes the rebound. All those quick carbs spike your blood sugar high, your pancreas pumps out insulin to deal with it, and two or three hours later? You crash again. Welcome to the blood sugar roller coaster, where you might end up eating way more throughout the day than your body actually needs.
I’ve talked to people who’ve gained 15-20 pounds in a year from this pattern alone, without changing anything else about their lifestyle.
Why Your Body Holds Onto Weight During Blood Sugar Drama

There’s another layer to this. Those stress hormones I mentioned? Cortisol, in particular, has a nasty habit of encouraging your body to store fat, especially around your midsection. When you’re experiencing frequent hypoglycemic episodes, you’re basically keeping your body in a low-grade stress state.
Chronic stress and cortisol also mess with your hunger hormones—ghrelin and leptin. Ghrelin tells you when you’re hungry, and leptin signals when you’re full. When these get out of whack, you might find yourself feeling hungry even after eating a decent meal.
People with diabetes face an extra challenge. Some folks deliberately keep their blood sugar running higher than ideal to avoid scary low episodes. But consistently elevated blood sugar can lead to weight gain over time, creating a lose-lose situation.
Breaking Free From the Low Blood Sugar Weight Trap
The good news? You’re not stuck with this forever. Small changes can break the cycle without making you feel deprived or scared of another crash.

First up: stop skipping meals. I know, I know—you’re busy, you’re not hungry in the morning, whatever. But eating breakfast within an hour of waking up sets the tone for stable blood sugar all day. It doesn’t need to be complicated. Greek yogurt with berries and nuts takes three minutes.
Balance is everything. Every meal should have protein, healthy fats, and fiber along with your carbs. This combo digests slowly and keeps your blood sugar steady for hours. Think of it as building a campfire versus throwing lighter fluid on kindling—you want sustained energy, not a quick flare-up.
When low blood sugar does hit, treat it smart. Keep glucose tablets or small juice boxes handy. Consume exactly 15 grams of fast-acting carbs, set a timer for 15 minutes, then reassess how you feel. Once you’re stable, have a small snack with protein to prevent another drop. This strategy stops the overcompensation habit.
Practical Eating Strategies That Actually Work

Snacking strategically makes a huge difference. If you go more than 4-5 hours between meals, you’re asking for trouble. Pack portable snacks like cheese and whole grain crackers, apple slices with peanut butter, or a handful of nuts with dried fruit.
Watch your carb choices. I’m not saying go low-carb or cut out bread forever. But there’s a real difference between white rice and brown rice, between Wonder Bread and sourdough. The fiber in whole grains slows down digestion and prevents those dramatic spikes and crashes.
Liquid calories deserve extra attention. Fruit juice, regular soda, and sweetened coffee drinks shoot your blood sugar up fast and bring it down just as quickly. They’re fine for treating actual hypoglycemia, but terrible as regular beverages.
When Professional Help Makes All the Difference
If you’re dealing with frequent low blood sugar episodes—more than a couple times a week—something deeper might be going on. Maybe your diabetes medications need adjusting. Perhaps you have reactive hypoglycemia or an insulin regulation issue that hasn’t been diagnosed yet.

Weight gain despite eating reasonably and exercising? That’s another red flag worth investigating. Thyroid issues, PCOS, and insulin resistance can all cause both blood sugar problems and unexplained weight changes.
A good endocrinologist can run proper tests and figure out what’s actually happening in your body. A registered dietitian who specializes in blood sugar management can create an eating plan that works for your real life, not some idealized version of it.
Getting Your Body Back on Track
Look, managing blood sugar while trying to maintain a healthy weight is genuinely challenging. Some days you’ll nail it, and some days you’ll eat half a box of crackers because you’re shaky and desperate. That’s being human.
The goal isn’t perfection. It’s creating enough stability that your body stops panicking and storing extra weight as insurance against the next crash. With consistent meal timing, balanced food choices, and appropriate treatment of low blood sugar when it happens, most people find their weight naturally stabilizes.
Your body wants to work with you, not against you. Give it the steady fuel it needs, and you might be surprised how much easier everything becomes.
Conclusion
Living with hypoglycemia doesn’t mean you’re destined to gain weight, but it does mean you need to be smarter about how you manage those blood sugar dips. The real culprit isn’t the low blood sugar itself—it’s the panic eating, the blood sugar roller coaster, and the stress hormones that come along for the ride.
Here’s what I want you to remember: your body is doing its best to protect you. Those intense cravings and that desperate hunger? They’re survival mechanisms, not personal failures. But you can work with your biology instead of fighting against it.
Start small. Eat breakfast tomorrow. Pack a balanced snack for mid-afternoon. When low blood sugar hits, treat it with exactly what you need—not everything within arm’s reach. These tiny shifts add up to major changes in how you feel and how your weight responds.
And please, if you’re struggling with frequent hypoglycemia or unexplained weight gain, talk to your doctor. You deserve answers and real solutions, not just a cycle of feeling crummy and watching your clothes get tighter.
Your relationship with food and your body doesn’t have to be this hard. With the right information and a bit of planning, you can stabilize your blood sugar and feel confident in your body again.
Frequently Asked Questions
Can low blood sugar make you gain belly fat specifically?
Yes, it can. The stress hormones released during hypoglycemic episodes—especially cortisol—tend to promote fat storage around your midsection. Frequent blood sugar crashes keep cortisol elevated, which signals your body to hold onto abdominal fat. This is why people dealing with chronic low blood sugar often notice weight gain primarily around their waist, even if they’re not overeating intentionally.
Why do I crave sweets so badly when my blood sugar drops?
Your brain runs almost entirely on glucose, so when blood sugar drops, it literally feels like an emergency. Your body releases adrenaline and other hormones that create intense cravings for quick sugar because that’s the fastest way to raise glucose levels. These aren’t psychological cravings you can willpower your way through—they’re biological survival signals. The key is responding with the right amount of fast-acting carbs rather than eating everything sweet in sight.
How long does it take to lose weight after stabilizing blood sugar?
This varies widely from person to person, but many people notice changes within 4-8 weeks of consistent blood sugar management. Once you break the cycle of crashes and overcompensation, your body stops holding onto extra weight as a protective measure. However, weight loss isn’t automatic—you still need to maintain a reasonable calorie balance. The difference is that with stable blood sugar, you’re not fighting constant hunger and cravings, making healthy eating feel much more manageable.
Is it better to eat small frequent meals or three larger ones for hypoglycemia?
For most people prone to hypoglycemia, eating three balanced meals with 1-2 planned snacks works better than constant grazing. The key is timing—try not to go more than 4-5 hours without eating something. Each meal should include protein, healthy fats, and complex carbs to provide sustained energy. Grazing on small amounts all day can actually keep your insulin levels elevated and make blood sugar harder to manage. Structure and balance matter more than frequency.
Can exercise help with hypoglycemia and weight management?
Exercise is definitely helpful, but timing matters. Regular physical activity improves insulin sensitivity and helps your body regulate blood sugar more effectively over time. However, exercising on an empty stomach or when your blood sugar is already low can trigger hypoglycemia. Have a small balanced snack 30-60 minutes before working out, and keep fast-acting carbs handy just in case. Once your blood sugar is more stable, exercise becomes one of your best tools for maintaining a healthy weight.

David Miller is a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. He creates clear, practical content to help readers make better everyday health choices.