What Level of Blood Sugar Is Dangerous? A Clear and Complete Guide
What level of blood sugar is dangerous? It’s one of the most important questions anyone managing diabetes — or worried about their glucose levels — can ask. And yet, so many people either don’t know the answer or have a vague sense of it without truly understanding what the numbers mean and when they signal a real emergency.
The truth is that both ends of the blood sugar spectrum carry serious risks. Blood sugar that climbs too high can damage your organs, trigger a life-threatening crisis, and cause long-term complications that affect nearly every system in your body. Blood sugar that crashes too low can impair brain function within minutes and, in severe cases, become fatal. Knowing exactly where the danger zones are — and what to do when you enter them — is knowledge that can literally save your life or the life of someone you love.
This guide lays it all out clearly, without confusing medical jargon or unnecessary complexity. Let’s get into the numbers.
Understanding Normal Blood Sugar Levels First
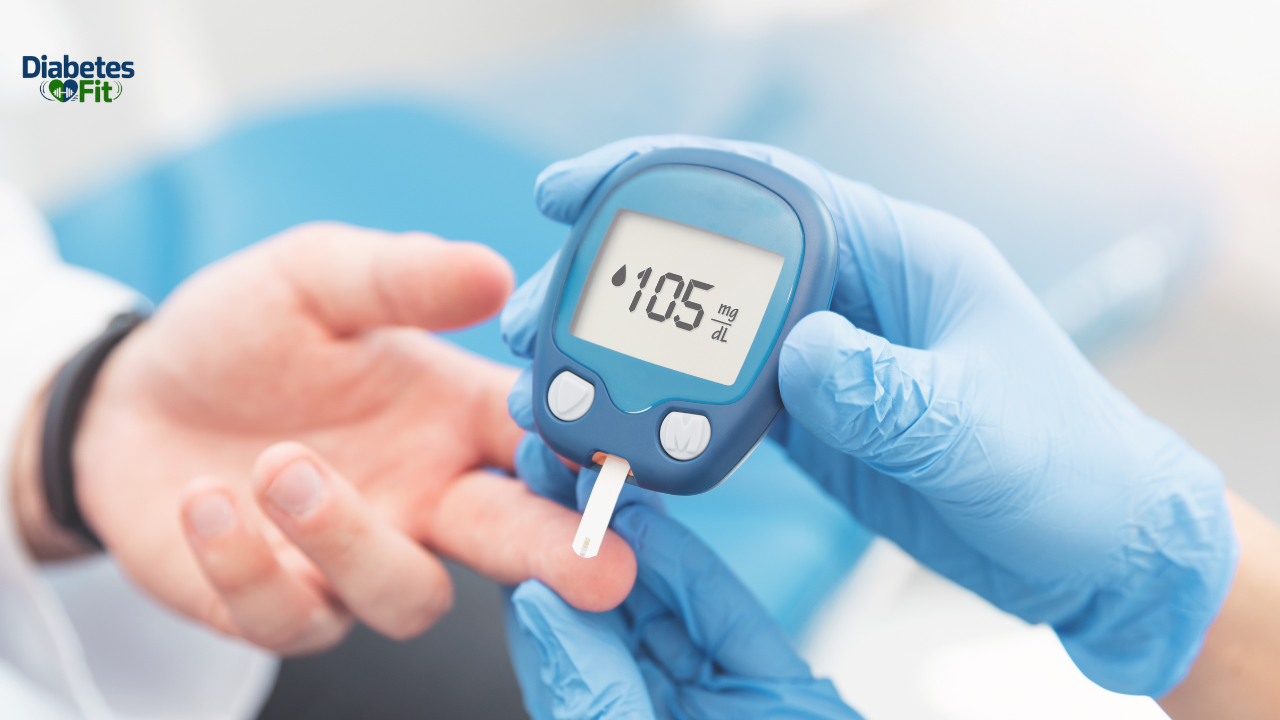
Before you can understand what’s dangerous, it helps to know what normal looks like. Blood sugar is measured in milligrams per deciliter (mg/dL) in the United States, or millimoles per liter (mmol/L) in most other countries. This guide will use mg/dL as the primary measurement.
For a person without diabetes, normal blood sugar levels generally fall within these ranges:
Fasting blood sugar (before eating, first thing in the morning) sits between 70 and 99 mg/dL. This is the healthy baseline your body returns to after an overnight fast.
After eating — typically measured two hours after a meal — blood sugar should ideally stay below 140 mg/dL. In truly healthy individuals, post-meal levels rarely exceed 120 mg/dL before returning to baseline.
The HbA1c test, which gives an average blood sugar picture over the past two to three months, should be below 5.7% in non-diabetic individuals.
For people with diagnosed diabetes, target ranges are slightly different and are set in collaboration with their healthcare provider. But the danger thresholds discussed in this article apply broadly, regardless of whether someone has a diabetes diagnosis.
What Level of Blood Sugar Is Dangerously High?
High blood sugar — medically called hyperglycemia — becomes increasingly concerning as levels climb above the normal range. Here’s how to think about the different thresholds.
Mildly elevated (140 to 180 mg/dL): Blood sugar in this range after meals may cause mild symptoms like increased thirst, frequent urination, and fatigue. While not immediately dangerous, regularly spending time in this zone causes cumulative damage to blood vessels and nerves over months and years.
Significantly elevated (180 to 250 mg/dL): At this level, symptoms become more noticeable. Blurred vision, headaches, difficulty concentrating, dry mouth, and tiredness are common. The kidneys are working hard to filter out excess glucose. For people with diabetes, readings consistently in this range indicate that management needs adjustment. For someone without diabetes, levels this high are a red flag worth investigating.
Dangerously high (250 to 350 mg/dL): This range is where things become acutely concerning. The risk of developing diabetic ketoacidosis (DKA) — a life-threatening complication — rises significantly. Symptoms at this level can include nausea, vomiting, abdominal pain, and a distinctive fruity smell on the breath caused by ketones building up in the bloodstream. Urgent medical attention is warranted.
Critical and emergency level (above 350 to 400 mg/dL): Blood sugar above 400 mg/dL is a medical emergency. At this level, the risk of DKA or hyperosmolar hyperglycemic state (HHS) — another potentially fatal complication — is extremely high. Confusion, extreme fatigue, rapid breathing, and even loss of consciousness can occur. Call emergency services immediately.
The American Diabetes Association recommends seeking medical attention if blood sugar reaches 300 mg/dL or above and is not responding to treatment, or at any level if symptoms of DKA or HHS are present.
Diabetic Ketoacidosis (DKA): What It Is and Why It’s Deadly
DKA is most commonly seen in people with type 1 diabetes, but it can also affect those with type 2 in certain circumstances. It happens when the body, starved of insulin and unable to use glucose for energy, begins breaking down fat at a dangerous rate. This produces acidic byproducts called ketones that accumulate in the blood, making it dangerously acidic.

Warning signs of DKA include fruity-scented breath, nausea and vomiting, stomach pain, rapid or labored breathing, extreme fatigue, and confusion. If untreated, DKA can progress to coma and death within hours to days.
Blood sugar at the onset of DKA is often above 250 mg/dL, but it’s important to note that ketone levels matter as much as blood sugar in this condition. Someone can develop DKA at blood sugar levels lower than 250 mg/dL in some circumstances, which is why testing for ketones is important when you’re feeling unwell and your blood sugar is elevated.
Hyperosmolar Hyperglycemic State (HHS): The Other High Blood Sugar Emergency
HHS is more common in older adults with type 2 diabetes and tends to develop more slowly than DKA, over days or even weeks. It occurs when blood sugar climbs to extremely high levels, often above 600 mg/dL, causing the blood to become very thick and concentrated.
Because HHS develops gradually, it can be easy to miss until the person is in serious trouble. Symptoms include extreme thirst, very frequent urination, confusion, vision changes, weakness, and, in severe cases, seizures or coma.
HHS has a higher mortality rate than DKA and requires immediate emergency medical treatment involving intravenous fluids and insulin. If someone you know — particularly an older adult — seems severely disoriented, unusually weak, or has been drinking and urinating excessively over several days, check their blood sugar and seek emergency care if levels are extremely elevated.
What Level of Blood Sugar Is Dangerously Low?
Low blood sugar — hypoglycemia — is equally dangerous and in some ways more immediately threatening because it can impair brain function rapidly. The brain runs almost exclusively on glucose, and when levels drop too low, it begins to malfunction within minutes.
Mildly low (70 mg/dL or below): This is the clinical threshold for hypoglycemia. Symptoms begin to appear around this level — shakiness, sweating, anxiety, rapid heartbeat, and hunger are the classic early warning signs. This level requires prompt treatment with fast-acting carbohydrates: glucose tablets, fruit juice, or regular soda.
Moderately low (54 to 70 mg/dL): Symptoms intensify. Difficulty concentrating, irritability, pale skin, and weakness are common. The “15-15 rule” is a common management strategy — consume 15 grams of fast-acting carbohydrates, wait 15 minutes, recheck levels.
Severely low (below 54 mg/dL): At this level, cognitive impairment becomes significant. The person may be unable to treat themselves, may become confused or combative, and may lose the ability to communicate clearly. Someone else needs to assist — this is when a glucagon emergency kit becomes essential.
Critical low (below 40 mg/dL): This is a full medical emergency. Seizures, loss of consciousness, and irreversible brain damage are possible at this level if not treated immediately. Call emergency services. If a glucagon kit is available and you know how to use it, administer it while waiting for help.
Who Is Most at Risk for Dangerous Blood Sugar Levels?
People with type 1 diabetes face the highest risk of both DKA and severe hypoglycemia, as their bodies produce no insulin at all, and glucose regulation is entirely dependent on external insulin management.
People with type 2 diabetes are at significant risk as well, particularly for hyperglycemic emergencies like HHS, especially if their condition is poorly managed, if they’re ill, or if they’re dehydrated.
People with undiagnosed diabetes are at particular risk because they have no monitoring system in place. Blood sugar can climb to dangerously high levels without anyone knowing until a crisis occurs.
Older adults face heightened risk because they may experience fewer or milder symptoms of both high and low blood sugar, meaning dangerous levels can go unnoticed longer.
Children with diabetes require especially careful monitoring because they may be unable to recognize or communicate symptoms effectively.
Warning Signs You Should Never Ignore
Certain symptoms should always prompt an immediate blood sugar check and potentially emergency action. These include sudden confusion or unusual behavior, extreme fatigue or weakness, vision changes, rapid or labored breathing, fruity breath odor, severe headache, seizures, loss of consciousness, uncontrollable shaking, and profuse sweating without physical exertion.
If blood sugar is tested and found to be below 54 mg/dL or above 300 mg/dL alongside any of these symptoms, treat it as a potential emergency. When in doubt, call for medical help. It is always better to make an unnecessary call than to wait too long during a true crisis.
Practical Steps to Avoid Dangerous Blood Sugar Levels
Monitoring regularly is the foundation of staying safe. People with diabetes should work with their healthcare provider to establish a testing schedule that catches dangerous trends before they become emergencies. Continuous glucose monitors (CGMs) have been transformative for many people, providing real-time data and alerts when levels move outside a safe range.

Keeping a consistent eating pattern, taking medications as prescribed, staying hydrated, carrying fast-acting glucose sources at all times, and wearing a medical ID bracelet are all practical measures that dramatically reduce risk.
Having an emergency plan — including who to call, where your glucagon kit is, and what instructions to give first responders — isn’t paranoid. It’s smart preparation.
Conclusion
What level of blood sugar is dangerous? The answer is clear once you know where to look. On the high end, levels above 300 mg/dL require urgent attention, and anything above 400 mg/dL is a medical emergency. On the low end, anything below 54 mg/dL is severely dangerous, and below 40 mg/dL demands immediate emergency intervention.
Understanding these thresholds, recognizing the warning signs, and knowing how to respond can make the difference between a manageable situation and a life-threatening crisis. Whether you’re managing diabetes yourself, caring for someone who is, or simply want to understand your own health better, these numbers are worth knowing by heart. Your awareness is one of the most powerful protective tools you have — use it.
FAQs
What blood sugar level should send you to the emergency room?
Generally, blood sugar above 300 mg/dL that isn’t responding to treatment — especially with symptoms like vomiting, confusion, or difficulty breathing — warrants emergency care. Levels above 400 mg/dL are always a medical emergency.
Is 200 mg/dL blood sugar dangerous?
A single reading of 200 mg/dL after eating may not be immediately dangerous, but it’s significantly elevated and should be addressed. Consistently high readings in this range cause long-term damage and increase the risk of serious complications.
What happens to your body when blood sugar is too high?
High blood sugar causes dehydration, damages blood vessels and nerves, strains the kidneys, and in severe cases triggers life-threatening conditions like DKA or HHS. Long-term hyperglycemia increases the risk of heart disease, kidney failure, blindness, and amputation.
Can low blood sugar be more dangerous than high blood sugar?
In the short term, yes. Severely low blood sugar can impair brain function, cause seizures, and lead to loss of consciousness within minutes. High blood sugar emergencies typically develop more slowly, giving slightly more time to respond — though both are serious.
What is a normal blood sugar level when you wake up?
A healthy fasting blood sugar upon waking should be between 70 and 99 mg/dL. Levels between 100 and 125 mg/dL may indicate prediabetes, while consistently above 126 mg/dL suggests diabetes and warrants medical evaluation.
Can stress cause dangerously high blood sugar?
Yes. Stress hormones like cortisol and adrenaline raise blood sugar levels. While stress alone rarely pushes levels into the emergency range in healthy individuals, it can be a significant factor for people with diabetes and can tip already-elevated levels into dangerous territory.

David Miller is a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. He creates clear, practical content to help readers make better everyday health choices.