What Causes Type 2 Diabetes? A Real, Honest Guide
The majority of people instantly associate “type 2 diabetes” with excessive sugar intake. To be honest, though, that is not the entire tale. My 54-year-old neighbor, who operated a small business, walked everywhere and hardly ever tasted sweets, was diagnosed.
His pancreas has been quietly battling for years, according to his doctor. I became aware of how little most of us truly know about the causes of type 2 diabetes at that very moment.
So let us have a proper conversation about it, using only the facts and not any jargon or scare tactics.
Healthy lifestyle habits can support both immunity and blood sugar control—read our post How to Boost Immune System Naturally to learn more.
What is Really Taking Place in Your Body?
Your body converts food into glucose, which powers your cells, each time you eat. However, glucose cannot enter your cells on its own. To function as a key that opens the cell door, it requires insulin, a hormone produced by the pancreas.
This functions flawlessly in a healthy body. After eating, blood sugar levels rise, insulin is released, glucose is absorbed by cells, and within a few hours, everything returns to normal.
This system malfunctions in type 2 diabetes in one of two ways, or both:
Insulin resistance is the inability of cells to react appropriately to insulin. The lock has changed, but the key is still there.
Beta cell exhaustion: The pancreas eventually loses its capacity to produce enough insulin after years of overwork.
Persistently elevated blood sugar is the outcome. And that gradually harms the heart, kidneys, blood vessels, nerves, and eyes.
So what is the first cause of type 2 diabetes? Let us go over it thoroughly.
1. Excess body fat, particularly in the abdomen
Being overweight in the stomach is one of the most well-known causes of type 2 diabetes. This is the bit that people overlook, though.
The problem is not the fat you can squeeze beneath your skin. The fat that is densely packed around your internal organs is called visceral fat. This fat has biological activity. It causes the release of inflammatory molecules that directly disrupt the way your cells react to insulin.
Imagine it as a steady, sluggish trickle of interference signals. Your cells become increasingly difficult to communicate with as you age. Blood sugar management begins to break down when insulin’s message is increasingly disregarded.
Because of this, waist circumference frequently predicts diabetes risk more accurately than total weight. Depending on where they store fat, two individuals may have the same BMI but very different metabolic risk levels.
Note: Regardless of overall body weight, a waist larger than 94 cm (37 inches) for men or 80 cm (31.5 inches) for women is associated with a markedly increased metabolic risk.
2. Physical Inactivity — The Silent Accelerator
Your muscles are your body’s largest consumers of glucose. When you move—walk, swim, climb stairs—muscles pull glucose directly from the bloodstream, often without even needing much insulin to do it. Exercise also makes your cells more sensitive to insulin for hours afterward.

When you’re largely sedentary, muscles become passive. They don’t demand glucose, so it accumulates in the blood. Combine that with a diet that keeps delivering glucose regularly, and you’ve got a slow but steady overload building in the system.
Here’s what surprises most people: even if you exercise for 30 minutes a day but sit for 8–10 hours, that long sitting window still causes real harm. Breaking up sitting time — even a 5-minute walk every hour — makes a documented, measurable difference.
3. What You Eat (And How Much of It Is Ultra-Processed)
Diet sits right at the center of what causes type 2 diabetes. But not in the oversimplified way people usually think.
Refined carbohydrates are the bigger issue
White bread, white rice, most breakfast cereals, crackers, and pastries—these break down almost instantly into glucose. Blood sugar spikes fast and hard. The pancreas scrambles to flood the system with insulin. Do this three to five times a day, every day, for years—and you’re exhausting the whole system. Eventually, cells start tuning out the repeated insulin signal.
Sugary drinks deserve special attention
Liquid sugar is uniquely harmful. A soda or sweetened juice delivers glucose almost immediately — no fiber, no protein, nothing to slow it down. Worse, drinks don’t trigger the fullness signals that solid food does. People consume enormous amounts of sugar without their bodies registering it.
Ultra-processed foods crowd out the good stuff
Packaged snacks, fast food, ready meals — these are calorie-dense, low in fiber, and engineered to keep you eating past fullness. They push out vegetables, beans, and whole grains that would otherwise slow digestion and keep blood sugar stable.
Worth knowing: A diet high in fiber—from vegetables, legumes, whole grains, and nuts—directly blunts blood sugar spikes after meals. Fiber slows glucose absorption the way brakes slow a car. Remove it, and that protection disappears.
4. Genetics and Family History
Here’s the part that makes some people uncomfortable: genetics genuinely matter when it comes to what causes type 2 diabetes.
If a parent or sibling has type 2 diabetes, your risk is meaningfully higher. If both parents had it, the risk roughly doubles. Genes influence how efficiently your pancreas produces insulin, how sensitive your cells are to it by default, and where your body tends to store fat.
But genetics is not destiny. People with a strong family history who stay active, eat well, and maintain a healthy weight can push their risk way down. The predisposition is real — but so is the ability to work against it.
5. Age and Declining Metabolic Function
The pancreas ages like every other organ. As people get older, insulin-producing beta cells become less efficient. Muscle mass tends to decline, reducing the body’s ability to absorb glucose. And fat tends to shift toward the abdomen, even in people whose total weight hasn’t changed much.
Risk climbs notably after age 45 and rises further after 60. But this isn’t a reason to accept it as inevitable. It’s a reason to be more proactive about diet, movement, and regular blood sugar checks during those decades.
One more thing worth saying: type 2 diabetes is no longer a condition that only affects older adults. It’s being diagnosed in growing numbers of people in their 20s and 30s, driven almost entirely by modern lifestyle changes.
6. Poor Sleep and Chronic Stress
These two causes of type 2 diabetes don’t get nearly the attention they deserve.

What poor sleep does to blood sugar
Even just a week of sleeping five or six hours a night measurably reduces insulin sensitivity in healthy people. Cortisol and growth hormone spike when you’re sleep-deprived—and both raise blood sugar. Your appetite hormones also shift: hunger goes up, and fullness signals go down. You eat more, and your body handles glucose worse. That combination does real damage over time.
How chronic stress feeds the problem
When you’re stressed, your body releases cortisol as part of the fight-or-flight response. Cortisol raises blood sugar — it’s designed to give you a quick burst of energy. Fine when the stressor is short-lived. But when stress is chronic—financial pressure, job burnout, relationship strain—cortisol stays elevated. Blood sugar stays chronically higher. Insulin gets called in constantly. Over the years, the system starts to wear down.
Chronic stress also disrupts sleep, reduces exercise, and triggers comfort eating. Rarely is it one thing alone — it’s usually everything compounding together.
7. Ethnicity and Biological Predisposition
Research consistently shows that certain ethnic groups develop type 2 diabetes at lower body weights. South Asian, East Asian, Middle Eastern, Hispanic, and African populations tend to face significantly elevated risk at BMIs that would be considered “normal” by standard Western charts.
This matters practically because standard BMI thresholds were developed using largely white European population data. For many groups, a BMI of 23 or 24 already carries real metabolic risk. This is one reason several countries now use lower BMI cutoffs for diabetes screening in these populations.
8. Other Medical Conditions That Raise Your Risk
Several health conditions are closely tied to what causes type 2 diabetes:
- Prediabetes — Blood sugar is elevated but not yet at the diabetic threshold. A critical window where lifestyle changes can reverse the trend.
- Polycystic ovary syndrome (PCOS) — Women with PCOS have elevated insulin resistance as part of their hormonal imbalance, significantly raising long-term diabetes risk.
- Gestational diabetes — Women who develop diabetes during pregnancy face roughly a 50% lifetime risk of developing type 2 diabetes later. A major warning sign.
- Non-alcoholic fatty liver disease (NAFLD)—The liver is central to glucose regulation. A fatty liver impairs this function and is strongly linked to insulin resistance.
- Certain medications—long-term use of corticosteroids, some antipsychotics, and specific blood pressure drugs—can reduce insulin sensitivity over time.
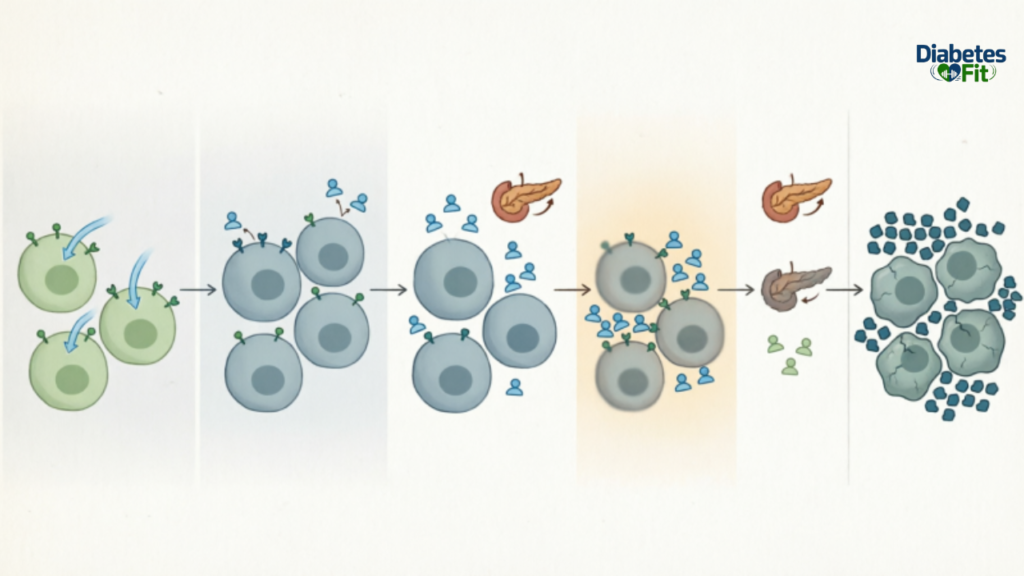
How Diabetes Type 2 Develops Over Time
One of the most confusing aspects of type 2 diabetes is how slowly it progresses. For the majority of people, it does not happen suddenly; rather, it develops gradually over years with little to no warning.
In general, this is what occurs:
Early insulin resistance is displayed by cells, but the pancreas makes up for it by making more insulin.
For a while, blood sugar remains normal, completely hiding the issue. As insulin resistance increases, the pancreas must work harder to keep up.
After meals, blood sugar begins to rise and remains elevated until it is unable to compensate.
The individual develops prediabetes, which is still treatable with the correct adjustments. Complete type 2 diabetes develops in the absence of intervention.
It may take five to fifteen years to complete this process. Fatigue, frequent urination, and blurred vision are examples of symptoms that frequently appear later. Because of this, routine blood sugar testing is crucial, particularly if you have any of the risk factors listed here.
Conclusion
Knowing the causes of type 2 diabetes alters your perspective on prevention. It has nothing to do with willpower or remorse. It involves a number of elements that subtly interact with one another, some inherited and some developed over years of everyday routines.
Fortunately, it is possible to actually control the majority of these elements. Early detection of increased blood sugar at the prediabetes stage provides a genuine window of opportunity to improve conditions before a final diagnosis.
You do not have to completely change your life in a single day. Walking more, getting better sleep, eating less processed food, controlling your stress, and getting your blood examined regularly—all of these adjustments, when made consistently over several months, yield tangible, quantifiable improvements. In actuality, biology responds to effort.
It is worth clinging to.
If you want to better understand how type 2 diabetes develops, this expert guide from Cleveland Clinic explains the causes clearly.
Frequently Asked Questions
Can you get type 2 diabetes if you’re not overweight?
Yes. Slim people can develop it—especially with a family history, physical inactivity, or belonging to a higher-risk ethnic group. Visceral fat (around organs) can be present even without visible weight gain.
Is sugar the main cause of type 2 diabetes?
Not exactly. Refined carbohydrates, excess calories, lack of movement, and body fat are bigger drivers overall. Sugary drinks are particularly problematic, but no single food causes diabetes on its own.
Can type 2 diabetes develop in young people?
Absolutely — and it’s happening more and more. While risk increases after 45, people in their 20s and 30s are increasingly being diagnosed, largely due to sedentary lifestyles and poor dietary habits.
Can type 2 diabetes be reversed?
For some people, yes — particularly when caught early. Significant weight loss and sustained dietary changes can lead to remission, where blood sugar normalizes without medication. The predisposition remains, so lifestyle habits need to be maintained.
Does stress actually cause type 2 diabetes?
Chronic stress is a real contributor. Cortisol raises blood sugar as part of the stress response. When that stress never goes away, blood sugar stays persistently elevated—and the cycle of poor sleep and overeating makes it worse.
What’s the difference between prediabetes and type 2 diabetes?
Prediabetes means blood sugar is elevated above normal but hasn’t crossed the clinical diabetes threshold yet. It’s the most important window for intervention—many people at this stage can fully reverse the trend with lifestyle changes before it becomes permanent.

David Miller: I am a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. I creates clear, practical content to help readers make better everyday health choices. I write evidence-based articles about diabetes, diet, and healthy living. My goal is to simplify complex health topics using trusted sources like WHO and medical journals.