What Causes Lower Back Pain in Females: 15 Reasons You Need to Know
Lower back pain is one of the most common health complaints among women worldwide — yet it’s also one of the most misunderstood. If you’ve been dealing with persistent or recurring back pain, you’re probably asking: What causes lower back pain in females specifically?
The answer is more complex than most people realize. While some causes of lower back pain affect everyone equally, women face a unique set of triggers — including hormonal fluctuations, reproductive health conditions, pregnancy, and menopause-related changes — that men simply don’t experience.
Understanding what causes lower back pain in females is the first step toward finding the right treatment, preventing future episodes, and knowing when a symptom needs urgent medical attention.
In this article, we cover 15 specific causes of lower back pain in women, warning signs to watch for, effective relief strategies, and clear answers to the most common questions. Let’s get into it.
Practicing gentle exercises like yoga can also help relieve back discomfort—check out our guide, Yoga to Reduce Belly Fat for Females at Home, for simple routines you can try.
Why Lower Back Pain Affects Women Differently
Before diving into specific causes, it’s important to understand why lower back pain in females deserves its own focused discussion.
Women’s bodies are anatomically and hormonally different from men’s in several key ways that directly affect the lower back:
- The female pelvis is wider, creating different angles of spinal loading and hip alignment
- Hormonal cycles — estrogen and progesterone fluctuations throughout the menstrual cycle affect ligament laxity, inflammation levels, and pain sensitivity
- Reproductive organs — the uterus, ovaries, and fallopian tubes are located in the pelvic area directly adjacent to the lower spine; conditions affecting these organs frequently cause referred lower back pain
- Pregnancy — dramatic structural and hormonal changes place unique stress on the lumbar spine
- Menopause — declining estrogen accelerates bone density loss and increases spinal vulnerability
- Higher rates of certain conditions — women are more likely than men to develop fibromyalgia, osteoporosis, autoimmune conditions, and endometriosis, all of which cause lower back pain
These differences mean that understanding what causes lower back pain in females requires looking beyond the spine itself to the full picture of women’s health.
What Causes Lower Back Pain in Females: 15 Common Causes
1. Muscle Strain and Ligament Sprain
How common: Most common cause in all adults. Pain type: Dull, achy, stiffness; worsens with movement
Muscle strain is the single most common answer to what causes lower back pain in females. It occurs when the muscles or ligaments supporting the spine are overstretched or torn — typically from:
- Lifting heavy objects incorrectly
- Sudden awkward movements
- Prolonged sitting with poor posture
- Overexertion during exercise
Key symptoms:
- Pain that worsens with bending, lifting, or twisting
- Muscle stiffness and tenderness to touch
- Spasms in the lower back muscles
- Pain that typically improves with rest
Treatment: Rest, ice for the first 48–72 hours, then heat, gentle stretching, anti-inflammatory medications, and gradual return to activity.
2. Poor Posture and Prolonged Sitting
How common: Extremely common, especially in office workers. Pain type: Chronic, dull ache that builds throughout the day

This is one of the most significant modern causes of lower back pain in females — driven by hours of desk work, phone use, and a sedentary lifestyle.
When you sit with poor posture — slouched forward, pelvis tucked under, head jutting forward — your lumbar spine loses its natural curve. This creates:
- Uneven pressure on spinal discs
- Shortening and tightening of the hip flexors
- Weakening of core muscles that support the spine
- Compression of spinal nerves
Key symptoms:
- Pain that builds throughout the day
- Relief when walking or moving
- Stiffness after getting up from sitting
- Headaches from associated neck tension
Prevention and treatment: Ergonomic workspace setup, regular movement breaks (stand up every 30–45 minutes), core strengthening, hip flexor stretching.
3. Menstrual Cycle and Dysmenorrhea
How common: Affects up to 80% of women at some point. Pain type: Cramping, lower back ache, radiating pain
Menstrual-related lower back pain is one of the most uniquely female causes — and one that many women dismiss as simply “normal period pain.” It’s one of the most important answers to what causes lower back pain in females that’s specific to women.
During menstruation, the uterus releases prostaglandins — hormone-like compounds that cause uterine contractions to shed the lining. High prostaglandin levels cause:
- Strong uterine contractions that radiate to the lower back
- Referred pain from the uterus to the lumbar region through shared nerve pathways
- Inflammation throughout the pelvic region
Key symptoms:
- Lower back pain that coincides with the first 1–3 days of menstruation
- Cramping in the lower abdomen and back simultaneously
- Nausea, fatigue, and headache accompany the pain
- Pain that improves after the first few days of the period
Treatment: NSAIDs (ibuprofen, naproxen) taken before cramping begins, heat therapy, gentle yoga, magnesium supplementation, and hormonal contraception for severe cases.
4. Endometriosis
How common: Affects 10–15% of women of reproductive age. Pain type: Severe, chronic, often debilitating — worsens before and during periods
Endometriosis is one of the most significant and underdiagnosed causes of lower back pain in females. It occurs when tissue similar to the uterine lining grows outside the uterus — on the ovaries, fallopian tubes, bowel, bladder, and sometimes directly on spinal nerves.
When endometrial implants are located near or on the sacral nerves or uterosacral ligaments, they cause severe, chronic lower back pain that many women mistake for a spinal problem.
Key symptoms:
- Severe lower back and pelvic pain that worsens dramatically before and during periods
- Pain during or after intercourse
- Painful bowel movements or urination during menstruation
- Heavy or irregular periods
- Infertility
- Pain that doesn’t respond well to standard pain medications
Diagnosis: Laparoscopy (minor surgery) is the gold standard for diagnosis. Ultrasound and MRI can identify larger lesions, but miss many cases.
Treatment: Hormonal therapies (birth control pills, progestins, GnRH agonists), pain management, and surgical removal of endometrial implants.
5. Premenstrual Syndrome (PMS) and PMDD
How common: PMS affects 75% of women; PMDD affects 3–8% Pain type: Lower back ache in the week before menstruation
PMS and its more severe form, PMDD (Premenstrual Dysphoric Disorder), cause lower back pain in the luteal phase — the week or two before menstruation begins.
The mechanism involves:
- Progesterone-driven fluid retention that causes pelvic congestion and pressure on spinal structures
- Increased prostaglandin sensitivity
- Hormonal fluctuations that lower the pain threshold
- Progesterone’s effect on ligament laxity temporarily destabilizes the sacroiliac joint
Key symptoms:
- Lower back ache that appears 7–14 days before the period
- Bloating, breast tenderness, and mood changes accompany the pain
- Complete resolution of pain after menstruation begins
6. Pregnancy
How common: 50–80% of pregnant women experience lower back pain. Pain type: Dull ache, sciatic pain, or sharp SI joint pain
Pregnancy is one of the most common and physically demanding causes of lower back pain in females. Multiple factors work together to stress the lower back during pregnancy:
- Weight gain — the growing uterus shifts the center of gravity forward, dramatically increasing lumbar lordosis (the inward curve of the lower back) and placing enormous pressure on the lower spine
- Relaxin hormone — released throughout pregnancy to loosen ligaments in preparation for childbirth, relaxin also destabilizes the sacroiliac joint and pubic symphysis
- Core weakness — as the abdomen expands, core muscles stretch and weaken, reducing spinal support
- Postural compensation — women naturally lean backward as their belly grows, compressing lower spinal structures
Key pregnancy-related back conditions:
- Lumbar lordosis pain
- Sacroiliac (SI) joint dysfunction
- Sciatica (nerve pain radiating down one or both legs)
- Pelvic girdle pain (symphysis pubis dysfunction)
Treatment: Prenatal yoga, maternity support belts, physical therapy, safe exercises like swimming and walking, and pregnancy-approved pain relief.
7. Sacroiliac Joint Dysfunction
How common: More common in women than men (due to wider pelvis and hormonal factors). Pain type: One-sided lower back pain, buttock pain, pain that worsens when standing on one leg
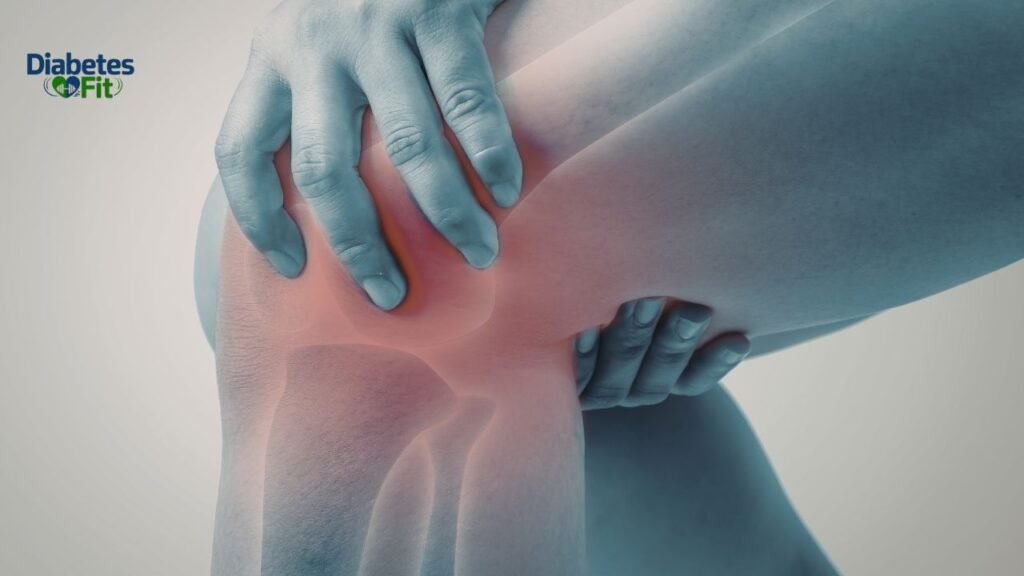
The sacroiliac (SI) joints connect the sacrum (base of spine) to the iliac bones of the pelvis. Women are significantly more prone to SI joint dysfunction than men because:
- The female pelvis is wider, creating a different force distribution through the SI joints
- Estrogen and relaxin make female ligaments more lax, reducing SI joint stability
- Pregnancy dramatically loosens the SI joint ligaments
- Hormonal changes during the menstrual cycle affect ligament tension
Key symptoms:
- Pain on one side of the lower back, just above the buttocks
- Pain that radiates into the buttock, groin, or thigh
- Pain that worsens when climbing stairs, walking uphill, or standing on one leg
- Stiffness in the morning that improves with movement
- Pain that worsens during pregnancy or around menstruation
8. Ovarian Cysts
How common: Most women develop at least one ovarian cyst in their lifetime. Pain type: Dull ache or sharp stabbing pain in one side of the lower back or pelvis
Ovarian cysts are fluid-filled sacs that form on or inside the ovaries. Since the ovaries are located in the lower pelvis, directly adjacent to the lumbar spine, cysts — especially large ones — can cause significant lower back and pelvic pain.
Key symptoms:
- Dull, aching lower back pain on one side (corresponding to the affected ovary)
- Pelvic fullness or pressure
- Pain during intercourse
- Irregular periods
- Sudden severe pain if a cyst ruptures — requires immediate medical attention
- Bloating and difficulty with bowel movements if the cyst is large
Red flag: Sudden, severe one-sided lower abdominal or back pain, fever, and vomiting may indicate a ruptured cyst or ovarian torsion — a medical emergency.
9. Uterine Fibroids
How common: Affects 20–80% of women by age 50. Pain type: Chronic pelvic pressure, lower back ache, heavy periods
Uterine fibroids are non-cancerous growths that develop in or on the uterus. They are one of the most common gynecological causes of lower back pain in females, particularly in women in their 30s and 40s.
Large fibroids or fibroids located on the back of the uterus press directly on spinal nerves and the lumbar region, causing:
- Chronic lower back and pelvic pain
- Pressure on the rectum, causing bowel changes
- Pressure on the bladder, causing frequent urination
- Heavy, prolonged menstrual bleeding
- Abdominal bloating
Treatment: Depends on size, location, symptoms, and desire for future pregnancy. Options include watchful waiting, medication, uterine fibroid embolization, myomectomy, or hysterectomy for severe cases.
10. Osteoporosis and Vertebral Fractures
How common: Affects 1 in 3 women over 50 Pain type: Sudden acute pain in one area of the spine, or chronic aching

Osteoporosis — the thinning and weakening of bones — is far more common in women than men, particularly after menopause when estrogen levels drop dramatically. Estrogen plays a critical role in maintaining bone density, and its loss accelerates bone resorption significantly.
In women with osteoporosis, vertebral compression fractures — tiny stress fractures in the spinal vertebrae — can occur with minimal trauma or even spontaneously. These are one of the most serious answers to what causes lower back pain in females in older women.
Key symptoms:
- Sudden, severe lower or mid-back pain after minimal exertion
- Loss of height over time
- Increasingly stooped posture (kyphosis)
- Back pain that worsens with standing or walking
- Pain that’s worse in certain positions
Risk factors: Family history, low calcium and vitamin D intake, small frame, smoking, excessive alcohol, long-term steroid use, early menopause.
Treatment: Calcium and vitamin D supplementation, bisphosphonate medications, weight-bearing exercise, fall prevention strategies.
11. Herniated or Bulging Disc
How common: Common across all adults; more likely after 30s Pain type: Sharp, shooting, or radiating pain — often down one leg
A herniated disc occurs when the soft inner material of a spinal disc pushes through its outer casing and presses on nearby nerves. In the lumbar spine, this frequently causes lower back pain that radiates down one leg — a condition called sciatica.
Women face specific risk factors for disc herniation:
- Hormonal changes that affect disc hydration and integrity
- Pregnancy-related spinal loading
- Rapid weight changes
- Osteoporosis-related vertebral changes
Key symptoms:
- Sharp, burning, or shooting pain from the lower back down one leg
- Numbness or tingling in the buttock, thigh, calf, or foot
- Weakness in the leg or foot
- Pain that worsens with sitting, bending, or sneezing
- Relief when walking or changing positions
12. Piriformis Syndrome
How common: Women are six times more likely than men to develop this condition. Pain type: Deep buttock pain that radiates down the leg, mimicking sciatica
The piriformis is a small muscle deep in the buttocks that runs from the sacrum to the hip. In many people, the sciatic nerve passes directly through or under the piriformis. When the piriformis becomes tight or inflamed, it compresses the sciatic nerve — causing lower back, buttock, and leg pain that closely mimics disc herniation.
Women are significantly more prone to piriformis syndrome because:
- The wider female pelvis creates a different angle of the piriformis muscle
- Hormonal changes affect muscle tension and flexibility
- Pregnancy-related pelvic changes affect piriformis mechanics
Key symptoms:
- Deep aching in the buttocks — often mistaken for hip or lower back pathology
- Pain that radiates from the buttocks down the back of the thigh
- Pain that worsens with sitting for prolonged periods
- Tenderness when pressing directly on the piriformis muscle
13. Kidney Infections and Kidney Stones
How common: Kidney infections are significantly more common in women than men. Pain type: One-sided flank pain, may radiate to the lower back
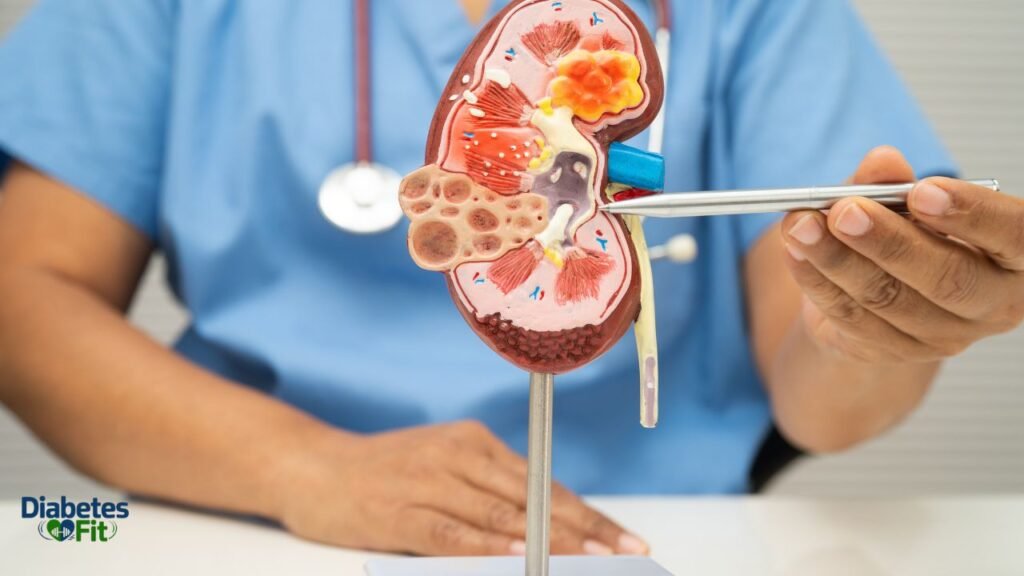
Women’s shorter urethra makes them far more susceptible to urinary tract infections (UTIs) that can ascend to the kidneys — causing pyelonephritis (kidney infection). Kidney stones are also a relatively common cause of lower back pain in females.
Both conditions cause pain in the flank and lower back area that is often mistaken for a musculoskeletal problem.
Key symptoms of kidney infection:
- One-sided lower back or flank pain (under the rib cage, above the waist)
- Fever and chills
- Nausea and vomiting
- Burning urination and frequent urge to urinate
- Cloudy or bloody urine
- General feeling of illness
Key symptoms of kidney stones:
- Sudden, severe, colicky one-sided pain that comes in waves
- Pain that radiates from the back to the lower abdomen and groin
- Blood in urine
- Nausea and vomiting
Red flag: Kidney infection with high fever requires urgent medical treatment with antibiotics. Untreated kidney infections can cause permanent kidney damage.
14. Scoliosis
How common: Adolescent idiopathic scoliosis is 8 times more common in girls than in boys. Pain type: Chronic uneven back pain, muscle fatigue, deformity-related pain
Scoliosis is an abnormal lateral curvature of the spine. While mild scoliosis is often painless in youth, it can become a significant source of lower back pain in females as they age — particularly during pregnancy (when hormonal changes affect spinal stability) and after menopause (when bone density decreases).
Key symptoms:
- Uneven shoulders or hips when standing
- One shoulder blade is more prominent than the other
- Chronic muscle fatigue and back pain on one side
- Rib prominence when bending forward
- Pain that worsens with prolonged standing or physical activity
15. Fibromyalgia
How common: 80–90% of fibromyalgia patients are women. Pain type: Widespread musculoskeletal pain, including lower back; heightened pain sensitivity
Fibromyalgia is a chronic condition characterized by widespread musculoskeletal pain, fatigue, sleep problems, and cognitive difficulties. The lower back is one of the most commonly affected areas, making fibromyalgia a significant cause of lower back pain in females that is often overlooked or misdiagnosed.
Key symptoms:
- Widespread pain in multiple body areas, including the lower back
- Extreme fatigue that doesn’t improve with rest
- Sleep disturbances — waking unrefreshed
- Brain fog (“fibro fog”) — difficulty concentrating
- Heightened sensitivity to pressure, temperature, and sound
- Depression and anxiety
Diagnosis: Clinical diagnosis based on widespread pain lasting more than 3 months, presence of tender points, and exclusion of other conditions.
Quick Reference: Causes of Lower Back Pain in Females
| Cause | Type of Pain | Other Key Symptoms | Who to See |
| Muscle strain | Dull, achy, stiffness | Worsens with movement | GP or physiotherapist |
| Poor posture | Builds through the day | Relief with movement | Physiotherapist |
| Menstrual pain | Cramping coincides with the period | Abdominal cramps | Gynecologist |
| Endometriosis | Severe, chronic, period-related | Painful sex, heavy periods | Gynecologist |
| Pregnancy | Dull ache, sciatica | Worsens as pregnancy progresses | OB/GYN, physiotherapist |
| SI Joint dysfunction | One-sided buttock pain | Worse on stairs | Physiotherapist |
| Ovarian cysts | One-sided, dull, or sharp | Pelvic fullness, irregular periods | Gynecologist |
| Uterine fibroids | Chronic pressure, heavy periods | Bloating, frequent urination | Gynecologist |
| Osteoporosis | Acute after minimal trauma | Height loss, stooped posture | Endocrinologist |
| Herniated disc | Sharp, radiates down the leg | Numbness, leg weakness | Spine specialist |
| Piriformis syndrome | Deep buttock pain | Worsens with sitting | Physiotherapist |
| Kidney infection | One-sided flank, fever | Fever, burning urination | Emergency/GP |
| Scoliosis | Uneven, chronic muscle fatigue | Uneven shoulders/hips | Orthopedic specialist |
| Fibromyalgia | Widespread, constant | Fatigue, sleep issues | Rheumatologist |
Warning Signs That Require Urgent Medical Attention
While the majority of female lower back pain is not harmful, some symptoms need to be evaluated by a doctor right away:

- Fever and sudden, intense lower back pain could be signs of a spinal or kidney infection.
- Cauda equina syndrome, a medical emergency requiring same-day surgery, may be indicated by lower back discomfort accompanied by numbness or weakness in both legs.
- Cauda equina syndrome emergency: loss of bladder or bowel control accompanied by back pain
- Following a fall or other trauma, lower back pain may indicate a fracture, particularly in older women.
- Back pain and unexplained weight loss necessitate a cancer screening.
- Severe, persistent pain that does not go away in any position requires immediate attention
- Gynecological assessment is necessary if you have back discomfort and vaginal bleeding outside of regular periods.
- Abrupt, intense one-sided pain accompanied by fever and vomiting could indicate a ruptured ovarian cyst or a renal problem.
How Lower Back Pain in Females Is Diagnosed
A proper diagnosis requires understanding the full picture — not just the spine. Your doctor may use:
| Diagnostic Tool | What It Shows |
| Physical examination | Range of motion, nerve function, and tenderness locations |
| X-ray | Bone structure, fractures, scoliosis, disc space narrowing |
| MRI | Soft tissues — discs, nerves, muscles, reproductive organs |
| Ultrasound | Ovarian cysts, uterine fibroids, and kidney abnormalities |
| Blood tests | Inflammation markers, kidney function, and hormonal levels |
| Laparoscopy | Definitive diagnosis of endometriosis |
| Bone density scan (DEXA) | Osteoporosis assessment |
| Urine analysis | Kidney infection, kidney stones |
Effective Treatments and Relief Strategies
Regarding Musculoskeletal Causes:
- Physical therapy and focused exercise (hip flexor stretching, core strengthening)
- Ice for acute injuries (initial 48–72 hours); heat therapy for persistent pain
- NSAIDs for pain and inflammation, such as naproxen and ibuprofen
- Chiropractic treatment and massage therapy
- Pilates and yoga for posture, strength, and flexibility
- Enhancements to the desk and sleeping posture that are ergonomic
Regarding Gynecological and Hormonal Causes:
- NSAIDs administered before the onset of menstrual discomfort (best effective when taken prophylactically)
- Hormonal contraception (lowers prostaglandin synthesis)
- Hormone treatment or surgery tailored to endometriosis
- Treatment for fibroids (medication, embolization, or surgery)
- Management of ovarian cysts (surgical excision or cautious waiting)
For Pain Associated with Pregnancy:
- Swimming and yoga during pregnancy
- Belts for maternity support
- Pregnancy-safe physical therapy
- Sleeping on your left side with a pillow between your knees is safe.
For Pain Associated with Osteoporosis:
- Supplementing with calcium and vitamin D
- Bisphosphonate drugs
- Exercise using weights to preserve bone density
- Techniques to prevent falls.
Frequently Asked Questions
What are the most common causes of lower back pain in females?
The most common causes of lower back pain in females include muscle strain and poor posture (affecting most women at some point), menstrual-related pain from prostaglandins, pregnancy-related structural and hormonal changes, sacroiliac joint dysfunction, endometriosis, uterine fibroids, ovarian cysts, and osteoporosis in older women. Women also experience herniated discs, piriformis syndrome, and kidney infections at significant rates. Understanding what causes lower back pain in females is important because many gynecological conditions cause back pain that may be mistaken for a spine problem.
When should I see a doctor for lower back pain as a female?
See a doctor promptly if your lower back pain is severe and sudden, accompanied by fever, associated with leg weakness or numbness, causes loss of bladder or bowel control, follows a fall or trauma, is accompanied by unexplained weight loss, or if you experience abnormal vaginal bleeding alongside the pain. These symptoms can indicate serious conditions, including cauda equina syndrome (emergency), kidney infection, ovarian cysts, or cancer that require prompt medical evaluation. Most lower back pain in females resolves within 4–6 weeks, but persistent pain beyond this should always be investigated.
Can hormonal changes cause lower back pain in females?
Yes — hormonal changes are one of the most significant and uniquely female causes of lower back pain. Estrogen and progesterone fluctuations throughout the menstrual cycle affect ligament laxity, inflammation levels, and pain sensitivity. Prostaglandins released during menstruation cause uterine contractions that radiate to the lower back. During pregnancy, relaxin loosens spinal ligaments. After menopause, declining estrogen accelerates bone density loss, increasing fracture risk. Understanding this hormonal connection is essential to fully understanding what causes lower back pain in females.
Can endometriosis cause lower back pain?
Yes — endometriosis is one of the most significant and frequently missed causes of lower back pain in females. When endometrial tissue grows near the sacral nerves, uterosacral ligaments, or bowel, it causes severe lower back pain that typically worsens dramatically in the week before and during menstruation. Many women with endometriosis-related back pain are misdiagnosed with a spinal condition for years before the true cause is identified. If your severe lower back pain consistently worsens with your period and doesn’t respond to standard treatments, ask your gynecologist about endometriosis.
Does lower back pain in females get worse with age?
Lower back pain in females tends to evolve with age rather than simply getting worse. In younger women, hormonal and menstrual causes predominate. During pregnancy, structural and hormonal changes are the primary drivers. After menopause, declining estrogen accelerates bone density loss (osteoporosis risk), increases degenerative disc disease, and removes the protective anti-inflammatory effects of estrogen, making spinal conditions more likely. However, many women find that menstrual-related back pain resolves or improves after menopause. Working with both a spine specialist and a gynecologist ensures all age-related causes are properly managed.
Can kidney problems cause lower back pain in females?
Yes — kidney infections (pyelonephritis) and kidney stones are significant causes of lower back pain in females and are much more common in women than men. Kidney pain typically presents as one-sided pain in the flank — the area below the rib cage and above the waist — rather than the central lower back pain of musculoskeletal causes. Kidney infection is accompanied by fever, chills, nausea, and urinary symptoms. Any lower back pain accompanied by fever, burning urination, or blood in urine requires urgent medical evaluation to rule out kidney pathology.
What exercises help reduce lower back pain in females?
The most effective exercises for lower back pain in females include core strengthening exercises (bird-dog, dead bug, plank), hip flexor stretches (low lunge, pigeon pose), glute strengthening (bridges, clamshells), pelvic tilts, cat-cow stretches, and gentle yoga. Swimming and walking are excellent low-impact options for women with pregnancy-related or osteoporosis-related back pain. Avoid high-impact activities during acute flare-ups. Physical therapy tailored to the specific cause of your lower back pain produces the best results — a physiotherapist can design a program addressing your individual anatomy and underlying cause.
Conclusion
Women’s lower back discomfort is rarely one-dimensional. Many women are coping with multiple contributing factors at the same time. The 15 causes discussed in this article vary from ordinary musculoskeletal problems to complicated hormonal and gynecological diseases.
Knowing what causes lower back pain in women gives you the ability to get the proper care at the right time from the right specialist. Whether your pain is caused by osteoporosis, endometriosis, menstrual prostaglandins, bad posture and muscle weakness, or pregnancy, particular, efficient treatments can significantly lessen or completely eradicate your discomfort.
Treating the incorrect cause of lower back pain in women costs time, delays relief, and may allow an underlying disease to worsen. Please do not delay if your back pain is severe, ongoing, or accompanied by any of the warning signals mentioned in this article.
Today, take the next action. Jot down your symptoms, including when the pain happens, what makes it better or worse, and whether it is related to your menstrual cycle or other changes in your health. Take this information to a women’s health professional or your physician. You are entitled to precise information, an accurate diagnosis, and a course of treatment that truly targets the underlying source of your suffering. It is worth it for your back and your quality of life.
If you want to better understand the reasons behind lower back pain in females, this helpful article fromHealthline explains it clearly.

David Miller: I am a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. I creates clear, practical content to help readers make better everyday health choices. I write evidence-based articles about diabetes, diet, and healthy living. My goal is to simplify complex health topics using trusted sources like WHO and medical journals.







