Why Does Blood Sugar Drop at Night? The Real Causes, Warning Signs, and How to Stop It
If you have ever woken up in a cold sweat, feeling shaky, confused, or with your heart pounding — and could not figure out why — there is a good chance your blood sugar dropped while you were sleeping. Understanding why blood sugar drops at night is one of the most important things a diabetic, prediabetic, or even a healthy person can know.
Nighttime low blood sugar, also called nocturnal hypoglycemia, is more common than most people realize, and it can happen silently while you sleep without obvious warning signals. It is not just uncomfortable — in some cases, it can be genuinely dangerous. In this article, you will learn exactly why blood sugar drops at night, who is most at risk, what the warning signs feel like, and most importantly, what you can do to prevent it. Let us break it down clearly, step by step.
Also read Cucumber Benefits for Diabetes.
What Is Nocturnal Hypoglycemia (Nighttime Low Blood Sugar)?
Before we answer why blood sugar drops at night, it helps to understand what is actually happening inside your body during a low blood sugar episode.
Hypoglycemia is the medical term for blood sugar that falls below normal levels. For most people, normal blood sugar ranges between 70 and 100 mg/dL (milligrams per deciliter) when fasting. Nocturnal hypoglycemia specifically refers to blood sugar dropping below 70 mg/dL during the nighttime hours — typically between midnight and 6 AM — while you are asleep.
The tricky part is that you are unconscious during these episodes. Your body tries to compensate and wake you up, but this does not always happen clearly or quickly enough. Some people sleep right through mild episodes. Others wake with severe symptoms. A small number experience what is called the “dead in bed” syndrome — an extremely rare but serious complication where severe undetected nocturnal hypoglycemia leads to cardiac events.
This is why knowing why blood sugar drops at night — and how to prevent it — genuinely matters.
Why Does Blood Sugar Drop at Night? The Main Causes Explained
There is rarely just one reason blood sugar drops at night. Most of the time, it is a combination of factors coming together in the nighttime hours when you cannot monitor yourself or make adjustments. Here are the most important causes, explained clearly.
1. Too Much Insulin Before Bed
This is the single most common reason why blood sugar drops at night, especially in people with Type 1 diabetes or insulin-dependent Type 2 diabetes. If your evening insulin dose — whether basal (long-acting) or bolus (fast-acting) — is slightly too high, it will continue lowering your blood sugar even after your last meal has been digested.
Fast-acting insulin peaks within 1 to 3 hours of injection. Long-acting insulin works more steadily but still has a peak activity period. If either type is overdosed relative to your carbohydrate intake and evening activity, the math works against you overnight.
Common insulin-related reasons for blood sugar drops at night include:
- Taking more rapid-acting insulin than needed for your evening meal
- Miscalculating your carbohydrate intake at dinner
- Using an insulin pen or pump that delivers slightly inconsistent amounts
- Not adjusting your basal dose after starting a new exercise routine
- Switching insulin brands or formulations without dose adjustment
2. Evening Exercise or Physical Activity
Exercise is one of the most powerful blood sugar-lowering forces your body has. Physical activity causes muscles to absorb glucose from the bloodstream for energy, and this effect does not stop the moment you finish your workout. In fact, your muscles continue drawing glucose from the blood for up to 12 to 24 hours after exercise to replenish their glycogen stores.

This means that if you exercise in the afternoon or evening, your body may still be in glucose-absorption mode when you fall asleep, which is a major reason why blood sugar drops at night after active days. This effect is particularly pronounced after:
- High-intensity interval training (HIIT)
- Long cardio sessions (running, cycling, swimming)
- Weightlifting or resistance training that depletes muscle glycogen
- Physical labor days when you were more active than usual
- Sports, games, or recreational activities done later in the day
3. Skipping or Eating a Light Dinner
Your evening meal is supposed to provide enough glucose to sustain your blood sugar through the night. When you eat a smaller dinner than usual, skip dinner entirely, or eat a very low-carbohydrate dinner, there simply is not enough glucose entering your bloodstream to maintain stable blood sugar during the fasting hours of sleep.
This is one of the reasons why blood sugar drops at night in people who are dieting aggressively, have poor appetite due to illness, or forget to eat properly before taking their evening medication or insulin.
4. Alcohol Consumption in the Evening
This one surprises many people. Alcohol initially raises blood sugar slightly because many alcoholic drinks contain carbohydrates (beer, wine, cocktails with mixers). But the real problem comes several hours later.

The liver’s primary job during fasting is to produce glucose through a process called gluconeogenesis — essentially creating glucose from stored glycogen to maintain your blood sugar while you sleep. Alcohol significantly impairs this process. When your liver is busy metabolizing alcohol, it cannot simultaneously produce glucose to maintain your blood sugar overnight. The result is a delayed blood sugar crash that often hits between 2 and 4 AM — well after the alcohol was consumed and any initial blood sugar effects have passed.
This is a major and underappreciated reason why blood sugar drops at night, especially in people who drink a moderate to large amount of alcohol in the evening without eating enough food alongside it.
5. Long-Acting Medication Effects
Beyond insulin, several common diabetes medications can cause blood sugar to drop at night:
- Sulfonylureas (glipizide, glibenclamide, glimepiride) — these stimulate the pancreas to produce insulin continuously, regardless of whether you have eaten. Their effects can persist overnight, especially longer-acting formulations.
- Meglitinides (repaglinide, nateglinide) — similar mechanism to sulfonylureas, though generally shorter-acting.
- Some newer combination medications — certain fixed-dose combination drugs contain multiple glucose-lowering agents that can compound overnight.
If you take any of these medications and are experiencing overnight blood sugar drops, your doctor may need to adjust your timing, dose, or formulation.
6. The Dawn Phenomenon (Paradoxically Causing Post-Drop Spikes)
While the dawn phenomenon primarily causes blood sugar to rise in the early morning hours, it is worth mentioning here because it is part of the overall overnight blood sugar picture.
Around 2 to 8 AM, the body releases hormones like growth hormone and cortisol to prepare for the day ahead. These hormones can cause blood sugar to rise. In some people, blood sugar first drops in the middle of the night (the Somogyi effect — explained below) and then rebounds dramatically as the dawn hormones kick in. This can mask the fact that a nighttime low occurred at all.
7. The Somogyi Effect (Rebound Hyperglycemia After Nocturnal Hypoglycemia)
The Somogyi effect — named after physician Michael Somogyi, who first described it — is a phenomenon where blood sugar drops at night and then rebounds to abnormally high levels as the body releases counter-regulatory hormones (glucagon, adrenaline, cortisol, and growth hormone) to correct the low.
People who experience the Somogyi effect often wake up with high blood sugar and blame it on overeating the night before, not realizing that their blood sugar actually dropped dangerously low during the night and their body overcompensated. This is one reason why understanding why blood sugar drops at night is important, even for people whose morning readings seem fine — or even high.
8. Poor Blood Sugar Control and Hypoglycemia Unawareness
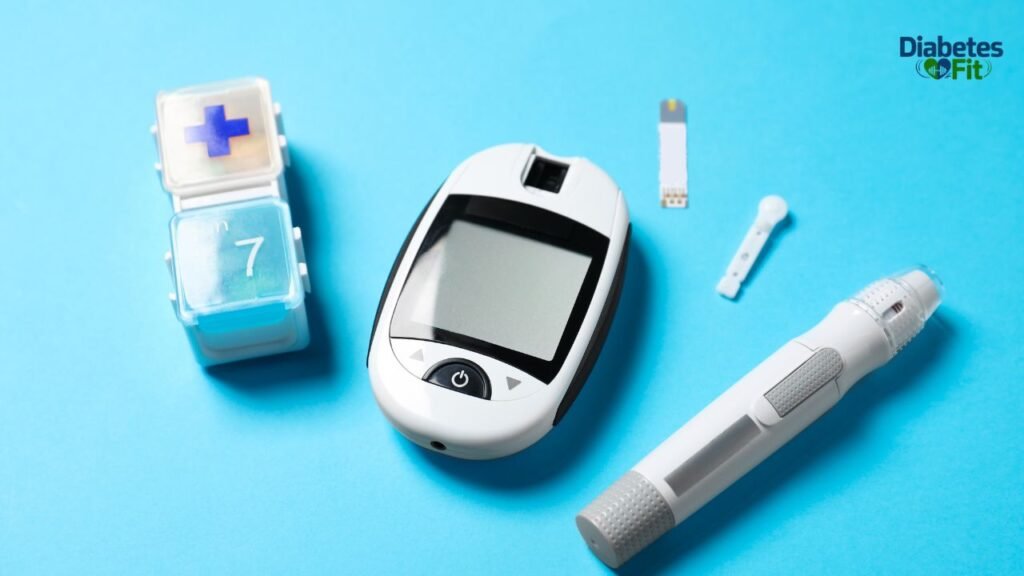
People who have had diabetes for many years, particularly those who have experienced frequent hypoglycemic episodes, can develop something called hypoglycemia unawareness. This means the body’s counter-regulatory hormonal response to low blood sugar becomes blunted over time. The early warning symptoms — shakiness, sweating, rapid heartbeat — that would normally wake a person up simply do not occur as reliably.
For these individuals, blood sugar can drop quite low during the night without triggering the alarm signals that would wake them. This makes monitoring and prevention especially critical.
Warning Signs That Blood Sugar Dropped at Night
Since you are asleep when nocturnal hypoglycemia occurs, the signs often show up as symptoms you notice upon waking or as disturbances in your sleep. Here is what to watch for:
During the Night:
- Waking suddenly, feeling anxious, shaky, or confused
- Night sweats or waking with damp sheets or clothing
- Nightmares or unusually vivid, disturbing dreams
- A rapid or pounding heartbeat that wakes you
- Difficulty getting back to sleep after waking abruptly
- Tingling or numbness in the lips, tongue, or fingers
- Crying out or talking in your sleep (reported by partners)
In the Morning (Signs Blood Sugar Dropped at Night While You Slept):
- Waking with a headache that was not there the night before
- Extreme fatigue or feeling unrested despite a full night of sleep
- Confusion, brain fog, or difficulty thinking clearly
- Nausea or upset stomach first thing in the morning
- Irritability or mood changes upon waking
- High morning blood sugar that seems unexplained (Somogyi rebound)
- Feeling like you need to eat immediately and urgently
Who Is Most at Risk for Nocturnal Hypoglycemia?
Not everyone is equally at risk of why blood sugar drops at night. The following groups face the highest risk:
| Risk Group | Key Reason for Elevated Risk |
| Type 1 Diabetics on Insulin | Continuous insulin action with no glucose intake during sleep |
| Type 2 Diabetics on Insulin | Same risk as Type 1, often compounded by longer duration of diabetes |
| People Taking Sulfonylureas | Continuous insulin stimulation regardless of food intake |
| Heavy Evening Exercisers | Prolonged glucose uptake by muscles post-exercise |
| People Who Drink Alcohol at Night | The liver’s glucose production is blocked by alcohol metabolism |
| Those with Hypoglycemia Unawareness | Counter-regulatory hormone response is blunted |
| Elderly Diabetics | Reduced counter-regulatory response, polypharmacy risk |
| Children with Type 1 Diabetes | Higher physical activity, growing bodies with variable glucose needs |
| People Who Skip or Eat Light Dinners | Insufficient glucose to sustain overnight blood sugar levels |
How to Prevent Blood Sugar from Dropping at Night
Now that you know why blood sugar levels fall at night and who is most vulnerable, let us discuss practical solutions. These are effective, realistic, and evidence-based tactics.
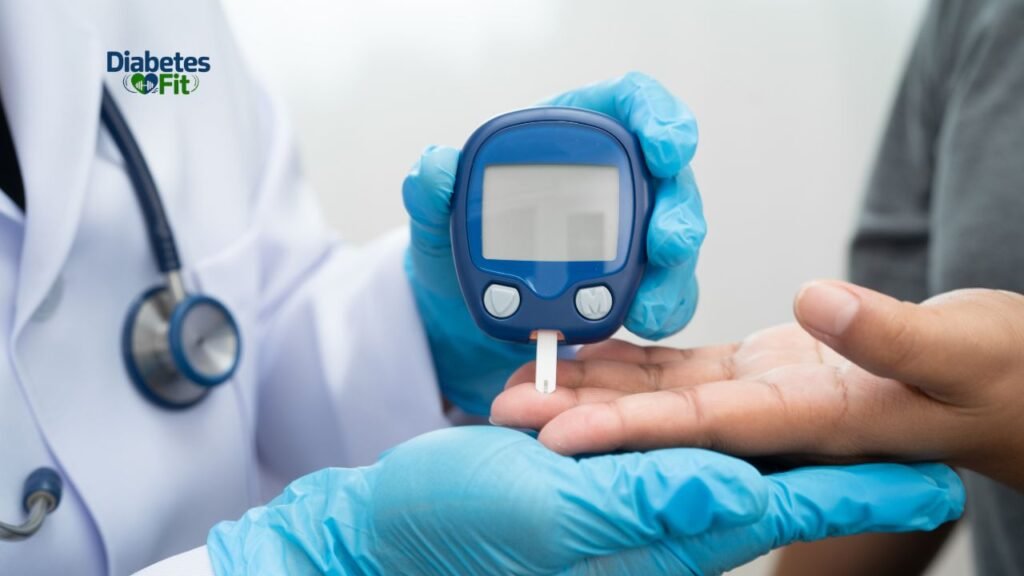
Consume a Wise Snack Before Bed
One of the best strategies to avoid blood sugar decreases during the night is to have a modest snack before bed that includes protein, fat, and slow-digesting carbohydrates. Giving your body a constant, gradual supply of glucose that lasts all night is the aim.
Some healthy options for a bedtime snack are:
- Almond or peanut butter-topped whole-grain crackers
- A handful of nuts and a tiny bowl of oats
- Whole-grain crackers and cheese
- Greek yogurt with a tiny bit of fruit
- A couple of whole-grain cookies and a hard-boiled egg
- A tablespoon of nut butter and a little apple
Aim for between 15 and 30 grams of complex carbohydrates combined with protein and fat, not a full meal, so avoid having a big, heavy snack.
Every night before going to bed, check your blood sugar.
This is necessary; it is not optional. Check your blood sugar before going to bed. Have a little snack if the level is less than 100 mg/dL. You are in a reasonable range if it is between 100 and 140 mg/dL, but keep a tight eye on it. If it is more than 180 mg/dL, ask your doctor if you need to change your insulin or evening medicine.
You may make an informed choice about whether to eat something before bed by knowing your pre-bed number. Knowing your pre-bed number gives you the information you need to make a smart decision about whether to eat something before sleeping.
Use Continuous Glucose Monitoring (CGM)
Continuous glucose monitors are game-changers for preventing nocturnal hypoglycemia. Devices like the Dexterity G7, FreeStyle Libre 3, and Medtronic Guardian continuously track your blood sugar every few minutes and send alerts to your phone or a receiver when levels drop below a set threshold. You can set an alarm to trigger if your blood sugar drops below 80 mg/dL during the night, waking you before the situation becomes dangerous.
If you are on insulin or taking medications that carry hypoglycemia risk, CGM is one of the most important investments you can make in your safety.
Adjust Insulin Timing and Dosing With Your Doctor
If you are consistently experiencing blood sugar drops at night, your insulin regimen likely needs adjustment. Do not make these changes on your own — work with your endocrinologist or diabetes care team. Common adjustments include:
- Reducing your basal insulin dose slightly
- Switching from a twice-daily long-acting insulin to a once-daily formulation
- Adjusting the timing of your evening bolus insulin relative to dinner
- Using an insulin pump with automated glucose-responsive insulin delivery
- Changing your evening medication to a formulation with a lower hypoglycemia risk
Adjust for Exercise on Active Days
On days when you exercise in the afternoon or evening, anticipate that your blood sugar may drop more overnight. Strategies include:
- Eating a larger or carbohydrate-rich dinner on exercise days
- Having a bedtime snack, even if you normally skip one
- Reducing your evening insulin dose on days of intense physical activity (discuss the specific reduction with your doctor)
- Checking blood sugar at 2 AM on nights after heavy exercise to see if you are experiencing a drop at that critical time
Reduce or Eliminate Evening Alcohol
Given how significantly alcohol impairs the liver’s ability to produce glucose overnight, reducing or eliminating alcohol — especially in the evening — is one of the most impactful changes you can make if you are prone to nighttime blood sugar drops. If you do drink alcohol, make sure you eat a full meal alongside it and have a bedtime snack before sleeping. Never go to bed with alcohol in your system and no food in your stomach.
Review All Medications With Your Doctor
If you take sulfonylureas or other medications known to cause hypoglycemia, ask your doctor whether the timing, dose, or formulation could be contributing to nighttime blood sugar drops. Some patients benefit from switching to medications with lower hypoglycemia risk (such as metformin, SGLT2 inhibitors, GLP-1 receptor agonists, or DPP-4 inhibitors) for their overnight coverage.
What to Do If You Wake Up with Low Blood Sugar at Night
If you wake up in the middle of the night and suspect your blood sugar has dropped, follow the 15-15 Rule:
- Check your blood sugar if you have a glucometer or CGM handy.
- If below 70 mg/dL, eat or drink 15 grams of fast-acting carbohydrates immediately:
- 4 glucose tablets
- 4 ounces (half a cup) of orange juice or apple juice
- 4 ounces of regular (not diet) soda
- 1 tablespoon of honey or corn syrup
- A small tube of glucose gel
- Wait 15 minutes, then check your blood sugar again.
- If still below 70 mg/dL, repeat step 2.
- Once blood sugar is above 100 mg/dL, eat a small snack of complex carbohydrates and protein to prevent another drop before morning.
- Tell your doctor about the episode the next day so your treatment plan can be reviewed.
Important: Keep glucose tablets, juice, or glucose gel on your nightstand so you can treat a low immediately without having to go to the kitchen.
Blood Sugar Targets at Night: What Numbers Should You Aim For?
| Time | Target Blood Sugar Range |
| Before bedtime | 100 to 140 mg/dL |
| 2 to 3 AM (if checking) | Above 90 mg/dL |
| Upon waking (fasting) | 80 to 130 mg/dL |
| Below this at any overnight point | Treat immediately as hypoglycemia |
These are general targets. Your doctor may set slightly different personal targets based on your age, diabetes type, duration, and risk of hypoglycemia unawareness. Always follow your care team’s specific guidance.
Frequently Asked Questions
Why does blood sugar drop at night even without diabetes?
Non-diabetic people can also experience nighttime blood sugar drops, though it is less common and rarely dangerous. Causes include reactive hypoglycemia (a blood sugar crash a few hours after a high-carb meal), prolonged fasting, strenuous exercise, excessive alcohol intake, or certain medical conditions like adrenal insufficiency or insulinoma. In otherwise healthy people, the body’s counter-regulatory hormones usually correct mild nighttime dips before they cause symptoms. If you frequently wake at night feeling shaky or sweating without a diabetes diagnosis, speak to your doctor about ruling out reactive hypoglycemia or other underlying causes.
What is the most dangerous time for blood sugar to drop at night?
The most vulnerable window is typically between 2 and 4 AM. This is when the counter-regulatory hormones that help raise blood sugar (glucagon and adrenaline) are at their lowest activity level, and when insulin action from evening doses may still be peaking. It is also the deepest phase of sleep for most people, making it harder to notice warning symptoms. If you are on insulin or sulfonylureas, checking your blood sugar at 2 to 3 AM periodically — or using a CGM with overnight alerts — gives you crucial information about whether your blood sugar drops at night during this high-risk period.
Can low blood sugar at night cause a seizure?
Yes, in severe cases. When blood sugar drops very low (typically below 40 to 50 mg/dL), the brain — which depends entirely on glucose for energy — begins to malfunction. This can progress from confusion to loss of consciousness and, in the most severe cases, seizures. This is a medical emergency. People who live alone and are at high risk for nocturnal hypoglycemia should consider CGM devices with external alarms, share their data with a family member or caregiver through connected apps, and discuss glucagon emergency kits with their doctor that can be administered by others if they are found unconscious.
Does blood sugar always drop at night in Type 1 diabetes?
Not always, but Type 1 diabetics are at significantly higher risk than the general population because they depend entirely on injected insulin with no natural pancreatic response to prevent overcorrection. The risk varies depending on basal insulin dose, evening eating habits, activity levels, and whether the person uses a closed-loop insulin pump system (artificial pancreas). Type 1 diabetics who use advanced closed-loop pump systems have considerably lower rates of nocturnal hypoglycemia because the system automatically adjusts insulin delivery based on real-time CGM readings.
Can stress cause blood sugar to drop at night?
Interestingly, psychological stress more commonly raises blood sugar rather than lowering it, because stress triggers the release of cortisol and adrenaline, which push glucose into the bloodstream. However, extreme physical exhaustion or the crash after a period of intense, sustained stress can sometimes contribute to a blood sugar dip. More relevant is the fact that poor sleep from stress can worsen insulin sensitivity over time, making blood sugar patterns less predictable. Addressing sleep quality and stress management is an important but often overlooked part of diabetes management.
How do I know if my morning high blood sugar is from the Somogyi effect?
The Somogyi effect and the dawn phenomenon can both cause high morning blood sugar, but they have different causes and require different treatments. To distinguish them, check your blood sugar between 2 and 3 AM for several nights in a row. If your 2 AM reading is low (below 70 mg/dL) and your morning reading is high, the Somogyi effect is likely — your blood sugar dropped at night and then rebounded. If your 2 AM reading is normal or slightly elevated and morning is high, the dawn phenomenon is more likely. These two conditions require opposite treatments, so accurate identification is essential — share your 2 AM readings with your doctor.
What should I eat before bed to stop my blood sugar from dropping at night?
The best bedtime snacks to prevent nighttime blood sugar drops combine slow-digesting complex carbohydrates with protein and a small amount of fat. This combination releases glucose slowly into the bloodstream over several hours, giving the body a steady fuel source while you sleep. Good choices include whole grain crackers with cheese or peanut butter, Greek yogurt with a few nuts, oatmeal with almond butter, or a hard-boiled egg with whole grain toast. Aim for around 15 to 25 grams of complex carbohydrates plus protein. Avoid simple sugars or fast-acting carbohydrates before bed as these digest too quickly and do not provide sustained overnight glucose coverage.
Conclusion
You regain control when you comprehend why blood sugar levels fall at night. It is not arbitrary. It is not erratic. It is caused by certain, identifiable factors that can be treated with the appropriate information and resources, such as excessive insulin, evening activity, alcohol, light food, and certain medications.
The main lessons are obvious. Before going to bed each night, check your blood sugar. When necessary, have a sensible bedtime snack. If your risk is high, use a continuous glucose monitor. Adjust your insulin and medicine dosages in close collaboration with your care team. On your nightstand, have fast-acting glucose. Additionally, take additional care on days when you exercise more or consume alcohol because you are more likely to experience a nocturnal blood sugar decrease.
You spend a third of your life sleeping, which is why it is important to you that blood sugar decreases at night. During those hours, your diabetes does not stop. However, you can make those nighttime hours just as secure and reliable as your waking ones with the correct routines, monitoring devices, and awareness.
Please let your doctor know at your next appointment if you commonly experience blood sugar dips at night. Do not wait. It is possible to control nocturnal hypoglycemia, but doing so requires treating it carefully. That discussion is important for your long-term health, safety, and sleep.
Medical Disclaimer: This article is for informational and educational purposes only. It does not constitute medical advice and should not replace consultation with a qualified healthcare professional. If you are experiencing blood sugar drops at night, speak with your doctor or diabetes care team promptly.
For more information, read the blog from the level.

David Miller is a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. He creates clear, practical content to help readers make better everyday health choices.







