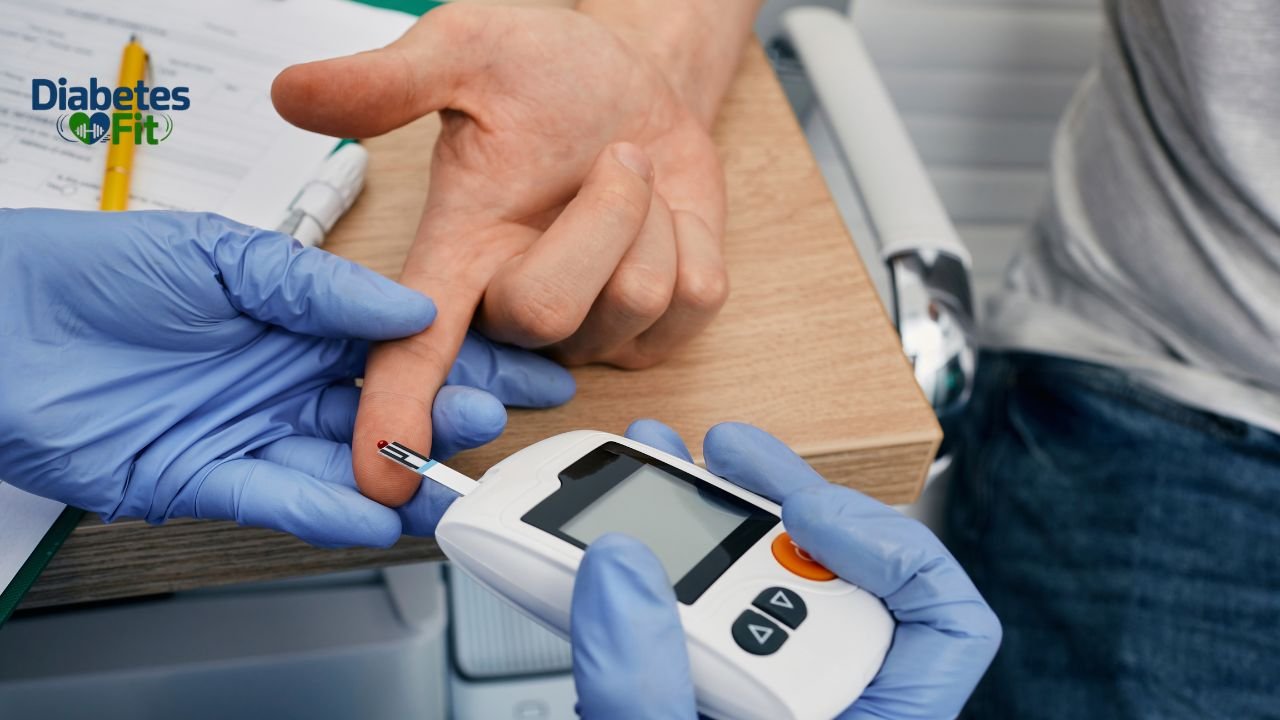
Can Fasting Cause Low Blood Sugar? You Need to Know Before You Skip Meal
Intermittent fasting is everywhere. Millions of people swear by it for weight loss, improved energy, and better metabolic health. But if you’ve ever skipped a meal and suddenly felt shaky, sweaty, dizzy, or strangely anxious — you already know that fasting isn’t always a smooth experience.
So can fasting cause low blood sugar? It’s one of the most important questions anyone considering intermittent fasting — or religious fasting — should understand before they start. And the honest answer is: yes, fasting can absolutely cause low blood sugar in certain people and under certain circumstances. But whether it happens to you depends on several important factors your doctor may never have mentioned.
This guide explains exactly how fasting affects blood glucose, who faces the highest risk, what hypoglycemia symptoms look like during a fast, and most importantly — how to fast safely without putting your health at risk. Whether you’re doing 16:8 intermittent fasting, a 24-hour fast, or religious observance fasting, this article is written for you.
You can read that Can Tirzepatide Cause Low Blood Sugar?
Can Fasting Cause Low Blood Sugar? The Biological Truth
To understand whether fasting causes low blood sugar, you first need to understand what normally keeps blood sugar stable when you’re not eating.
How Your Body Manages Blood Sugar During a Fast
Your body is remarkably good at maintaining blood glucose within a narrow range — even when you haven’t eaten in many hours. It does this through two main mechanisms:
1. Glycogenolysis — Breaking Down Stored Glucose
When you stop eating, your blood sugar begins to slowly fall. Your pancreas detects this and reduces insulin secretion. At the same time, it releases glucagon — a hormone that signals the liver to break down glycogen (stored glucose) and release it into the bloodstream. Your liver stores enough glycogen to keep blood sugar stable for approximately 12–16 hours of fasting in most healthy adults.
2. Gluconeogenesis — Making New Glucose
Once liver glycogen is depleted — typically after 12–24 hours of fasting — your body shifts to gluconeogenesis: manufacturing new glucose from non-carbohydrate sources like amino acids (from protein), lactate, and glycerol (from fat breakdown). This process keeps blood sugar from dropping dangerously low even during extended fasts.
In healthy people with normal hormonal function, these two systems work together efficiently enough that fasting does not typically cause clinically dangerous hypoglycemia. Blood sugar may drop toward the lower end of normal — perhaps 65–75 mg/dL — but the body’s counter-regulatory hormones (glucagon, cortisol, epinephrine, and growth hormone) prevent a dangerous crash.
So When Does Fasting Cause Low Blood Sugar?
Fasting causes low blood sugar when this regulatory system is disrupted — either because:
- A medication is forcing insulin production regardless of blood sugar levels
- The liver cannot release stored glucose properly
- Counter-regulatory hormones (glucagon, cortisol) aren’t responding adequately
- The person has an underlying metabolic condition that impairs glucose regulation
- The fast is extremely prolonged and the body can’t compensate fast enough
This is why can fasting cause low blood sugar is a question with a nuanced answer: it depends entirely on the individual’s health status, medications, and the type of fast being done.
Who Is Most at Risk for Low Blood Sugar During Fasting?
Understanding your personal risk level is the most important step before starting any fasting protocol.
People With Type 1 Diabetes
Type 1 diabetes means the pancreas produces little or no insulin. People with type 1 diabetes manage blood sugar with external insulin injections or an insulin pump. During fasting, if insulin doses are not carefully reduced, the injected insulin continues driving blood sugar down even without food — creating a serious, potentially life-threatening hypoglycemic episode.
Fasting with type 1 diabetes is possible but requires very careful medical supervision and real-time glucose monitoring — ideally with a continuous glucose monitor (CGM).
People With Type 2 Diabetes on Insulin or Sulfonylureas
People with type 2 diabetes taking insulin or sulfonylureas (glipizide, glibenclamide, glimepiride, glyburide) face significant hypoglycemia risk during fasting. Sulfonylureas stimulate insulin release regardless of blood sugar levels — they don’t have the glucose-dependent safety mechanism of newer medications. Fasting while on these drugs without dose adjustment creates a mismatch: the medication keeps pushing insulin, but no food is coming in to raise blood sugar.
In contrast, people with type 2 diabetes on metformin, SGLT2 inhibitors, or DPP-4 inhibitors have very low hypoglycemia risk during fasting, since these medications don’t directly stimulate insulin release.
People With Reactive Hypoglycemia
Reactive hypoglycemia is a condition where blood sugar drops too low — typically 2–4 hours after eating — in response to the body releasing too much insulin after a meal. This usually happens postprandially (after food), not during a fast. However, people with reactive hypoglycemia often have underlying insulin sensitivity issues that can make fasting blood sugar drops more pronounced.
People With Adrenal Insufficiency
The adrenal glands produce cortisol — a counter-regulatory hormone that raises blood sugar during fasting by stimulating gluconeogenesis. People with Addison’s disease or adrenal insufficiency lack adequate cortisol production. Without this hormonal protection, blood sugar can fall significantly during prolonged fasting. This group faces serious hypoglycemia risk and should fast only under close medical supervision.
People With Liver Disease
Since the liver is the primary organ responsible for releasing stored glucose and manufacturing new glucose during fasting, significant liver disease (cirrhosis, severe fatty liver disease, hepatitis) impairs the body’s ability to maintain blood sugar during a fast. Fasting-induced hypoglycemia is a recognized complication in people with advanced liver disease.
Children and Adolescents
Children have smaller glycogen stores relative to their body size and higher metabolic rates than adults. This means they deplete liver glycogen faster and are more vulnerable to fasting hypoglycemia — especially young children. Extended fasting is generally not recommended for children without medical oversight.
People Who Are Malnourished or Have Very Low Body Weight
People with very little body fat and muscle mass have smaller glycogen reserves and less substrate for gluconeogenesis. This limits the body’s ability to maintain blood sugar during extended fasting.
Risk Level Summary by Patient Type
| Person Type | Fasting Hypoglycemia Risk | Key Reason |
| Healthy adults — no medications | Very Low | Liver glycogen + gluconeogenesis maintain glucose |
| Type 2 diabetes — metformin only | Low | Metformin doesn’t directly lower blood sugar |
| Type 2 diabetes — SGLT2 inhibitors | Low | Glucose-independent mechanism |
| Type 2 diabetes — sulfonylureas | High | Insulin forced regardless of glucose level |
| Type 2 diabetes — insulin | High | Exogenous insulin drives glucose down |
| Type 1 diabetes — any insulin | Very High | Total insulin dependence + no self-regulation |
| Adrenal insufficiency | High | No cortisol counter-regulation |
| Liver disease (severe) | Moderate–High | Impaired glycogenolysis and gluconeogenesis |
| Children under 12 | Moderate | Small glycogen stores, high metabolic rate |
| Healthy people — 16:8 IF | Very Low | Short enough fast for liver glycogen to compensate |
What Does Low Blood Sugar Feel Like During Fasting?
Recognizing fasting-induced hypoglycemia early is critical. Many symptoms of low blood sugar overlap with how fasting normally feels in the first few days — hunger, mild dizziness, slight fatigue. But true hypoglycemia has a distinct pattern and intensity.

Mild Hypoglycemia Symptoms (Blood Sugar 54–70 mg/dL)
These are the early warning signs. They appear quickly and should prompt immediate treatment:
- Sudden, intense shakiness or trembling
- Cold sweats — breaking into a sweat without physical exertion
- Heart racing or pounding (palpitations)
- Sudden anxiety or feeling of dread
- Pale skin
- Strong, sudden hunger — different from the background hunger of fasting
- Lightheadedness or dizziness
- Difficulty concentrating — mind suddenly going blank
Moderate Hypoglycemia Symptoms (Blood Sugar 40–54 mg/dL)
At this level, cognitive function begins to deteriorate. These symptoms require immediate treatment — this is not the time to “push through”:
- Confusion or disorientation
- Slurred speech
- Blurred or double vision
- Emotional instability — crying, irritability, unusual aggression
- Weakness in arms or legs
- Difficulty walking or standing
Severe Hypoglycemia (Blood Sugar Below 40 mg/dL)
This is a medical emergency:
- Seizures
- Loss of consciousness
- Complete inability to swallow — never give food or liquid to someone unconscious
- Call emergency services immediately
Important distinction: Normal fasting symptoms — mild hunger, mild fatigue, slight headache in the first 1–2 days — are not the same as hypoglycemia. True hypoglycemic symptoms are sudden in onset, more intense, and often accompanied by physical signs like sweating and shakiness.
How Low Does Blood Sugar Drop During Fasting?
Here’s what the research actually shows about blood glucose levels during various fasting periods in healthy, non-diabetic people:
| Fasting Duration | Typical Blood Sugar Range | What’s Happening |
| 0–8 hours | 80–100 mg/dL | Normal post-absorptive state |
| 8–16 hours | 70–90 mg/dL | Liver glycogen releasing glucose steadily |
| 16–24 hours | 65–80 mg/dL | Glycogen depleting; gluconeogenesis beginning |
| 24–48 hours | 60–75 mg/dL | Full gluconeogenesis; ketone production rising |
| 48–72 hours | 55–70 mg/dL | Deep ketosis; brain adapting to use ketones |
| 72+ hours | 45–65 mg/dL | Extended fast; stable but at lower setpoint |
Notice that even during extended fasting, healthy people rarely drop below 55 mg/dL — the clinical threshold for significant hypoglycemia. The body’s regulatory systems keep blood glucose in a functional range.
People who experience hypoglycemia below 54 mg/dL during fasting almost always have an underlying factor — medication, hormonal imbalance, or metabolic condition — driving it.
Types of Fasting and Their Hypoglycemia Risk
Not all fasting is the same. Different fasting protocols carry significantly different risk levels.

Intermittent Fasting (16:8 Method)
The 16:8 method — eating within an 8-hour window, fasting for 16 hours — is the most popular form of intermittent fasting. For healthy adults without diabetes medications, the risk of low blood sugar during a 16-hour fast is very low. The liver’s glycogen stores are more than sufficient to cover this period.
Risk level for healthy adults: Very Low
24-Hour Fasting (One Meal a Day / OMAD)
A 24-hour fast is more demanding but still manageable for healthy adults. Blood sugar typically drops to the lower end of normal (65–75 mg/dL) but rarely reaches dangerous hypoglycemic levels without medication involvement.
Risk level for healthy adults: Low
Religious Fasting (Ramadan, Yom Kippur, etc.)
Religious fasting — particularly Ramadan, which involves complete abstinence from food and water from sunrise to sunset (typically 12–17 hours depending on location and season) — is widely practiced by hundreds of millions of people with diabetes. The combination of no food, no water (dehydration worsens hypoglycemia), and unchanged diabetes medications creates meaningful risk for those on insulin or sulfonylureas.
Multiple medical guidelines specifically address fasting during Ramadan for people with diabetes, recommending pre-Ramadan medication adjustments and frequent blood glucose monitoring. Always consult your doctor at least 4–6 weeks before Ramadan if you have diabetes.
Risk level for diabetics on insulin/sulfonylureas: High without medication adjustment
Extended Fasting (48–72+ Hours)
Extended fasting significantly increases hypoglycemia risk — particularly for people with any underlying metabolic or hormonal condition. Even healthy people undergoing extended fasts should monitor blood sugar and have fast-acting carbohydrates available. Extended fasting without medical supervision is not recommended for people on diabetes medications.
Risk level: Moderate for healthy adults; High for anyone on blood-sugar-lowering medications
How to Fast Safely and Prevent Fasting-Induced Low Blood Sugar
Whether you’re doing intermittent fasting for weight loss or observing religious fasting, these strategies significantly reduce your risk of dangerous hypoglycemic episodes.
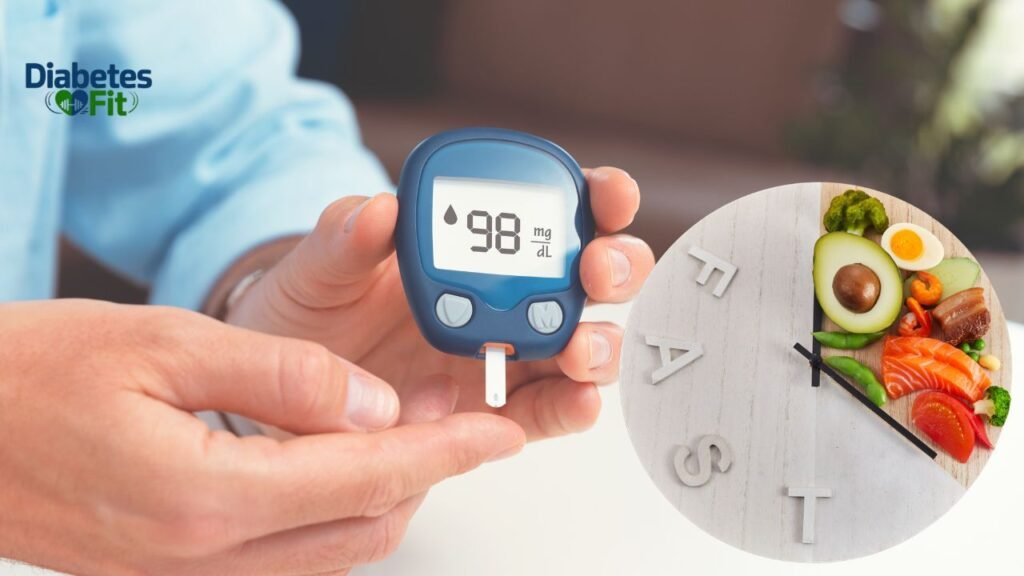
1. Talk to Your Doctor Before Starting Any Fast
If you take any diabetes medication — insulin, sulfonylureas, even GLP-1 agonists like semaglutide or tirzepatide — speak to your doctor before fasting. Doses almost certainly need adjustment. Never self-adjust insulin or other diabetes medications without medical guidance.
2. Monitor Your Blood Sugar Frequently
During any fast longer than 12 hours, check your blood sugar:
- Before breaking your fast
- During the fasting window if you feel symptomatic
- 1–2 hours after eating when you break the fast
A continuous glucose monitor (CGM) eliminates the need for most manual checks and provides real-time alerts — making fasting significantly safer for people with diabetes.
3. Break Your Fast Immediately If Blood Sugar Drops Below 70 mg/dL
At 70 mg/dL with symptoms — don’t push through. Break your fast. Use the 15-15 Rule:
- Take 15 grams of fast-acting carbohydrates (3–4 glucose tablets, 4 oz juice, 1 tablespoon of honey)
- Wait 15 minutes
- Recheck blood sugar
- If still below 70 mg/dL — repeat
- Once above 70 mg/dL — eat a small balanced meal
4. Stay Well Hydrated During Fasting
Dehydration worsens hypoglycemia symptoms and impairs the body’s counter-regulatory responses. During fasting periods, drink water consistently. Electrolyte water (without sugar) or plain herbal tea are also good options.
5. Eat a Balanced Pre-Fast Meal
The meal before your fasting window starts matters more than most people realize. A meal rich in:
- Complex carbohydrates (oats, brown rice, legumes) — slow glucose release
- Lean protein (eggs, chicken, lentils) — supports gluconeogenesis
- Healthy fats (avocado, nuts, olive oil) — slows digestion further
…will sustain blood sugar for significantly longer into your fast than a meal of refined carbs.
6. Avoid Intense Exercise During Extended Fasts
Exercise lowers blood sugar by increasing glucose uptake in muscles. Combining intense exercise with extended fasting — especially if on diabetes medications — significantly increases hypoglycemia risk. If you exercise during a fast, keep it light (walking, gentle yoga) and monitor your blood sugar closely.
7. Always Carry Glucose Tablets
If you have any risk factors for hypoglycemia — diabetes medications, adrenal insufficiency, history of low blood sugar — glucose tablets should be on your person at all times during a fast. They provide the fastest, most precise treatment for mild hypoglycemia and can prevent a mild episode from becoming a dangerous one.
Fasting Blood Sugar Levels: What’s Normal, What’s Concerning
| Fasting Blood Sugar | Classification | Action Needed |
| Above 100 mg/dL | Normal to Prediabetic Range | Monitor; no immediate action |
| 80–100 mg/dL | Normal fasting range | No action needed |
| 70–79 mg/dL | Low-normal; watch for symptoms | Monitor closely |
| 54–69 mg/dL | Mild hypoglycemia | Treat with 15g fast-acting carbs immediately |
| 40–53 mg/dL | Moderate hypoglycemia | Treat immediately; consider breaking fast |
| Below 40 mg/dL | Severe hypoglycemia | Emergency — call for help immediately |
Frequently Asked Questions
Can intermittent fasting cause low blood sugar in non-diabetic people?
In healthy, non-diabetic people without underlying hormonal conditions, standard intermittent fasting (16:8 or even 24-hour fasting) very rarely causes dangerously low blood sugar. Blood glucose may drop to the lower end of normal (65–75 mg/dL), which can cause mild symptoms like hunger and slight dizziness — but true hypoglycemia (below 54 mg/dL) in healthy people during typical IF protocols is uncommon. If it does occur repeatedly, it warrants investigation for reactive hypoglycemia or other underlying conditions.
How long does it take for blood sugar to drop dangerously during fasting?
In healthy adults, blood sugar remains in a safe range for 12–24+ hours of fasting thanks to liver glycogen and gluconeogenesis. Dangerous drops typically occur much faster — within a few hours — only in people on insulin or sulfonylureas who haven’t adjusted their doses. Without those medications, the body’s regulatory systems are generally capable of preventing dangerous hypoglycemia for extended periods.
What should I eat to prevent low blood sugar during fasting?
The pre-fast meal makes the biggest difference. Eat a combination of complex carbohydrates (oats, sweet potato, brown rice, lentils), lean protein (eggs, chicken, fish), and healthy fats (avocado, nuts, olive oil). This combination provides sustained, slow-release energy that extends blood sugar stability well into your fasting window — far more effectively than a meal of refined carbs, which spikes and crashes within 2 hours.
Is it safe for diabetics to do intermittent fasting?
It depends on the medications and the type of diabetes. People with type 2 diabetes on metformin, SGLT2 inhibitors, or lifestyle management alone can often do intermittent fasting safely with their doctor’s guidance. People on insulin or sulfonylureas face significant hypoglycemia risk during fasting and need medication dose adjustments before starting. People with type 1 diabetes should only fast under close medical supervision with real-time glucose monitoring. Always discuss fasting with your diabetes care team before starting.
What is the difference between fasting hunger and low blood sugar?
Fasting hunger is gradual, builds slowly, and is typically accompanied by a grumbling stomach. It improves temporarily when you drink water and doesn’t include physical signs like sweating or shakiness. Hypoglycemia comes on suddenly and intensely — typically with shaking, cold sweating, heart pounding, sudden intense anxiety, and dizziness — and it does not improve with water alone. If you experience these sudden physical symptoms during a fast, check your blood sugar and treat if below 70 mg/dL — don’t assume it’s just hunger.
Can drinking only water during fasting prevent low blood sugar?
Water does not prevent or treat low blood sugar — it contains no glucose or carbohydrates. However, staying well hydrated during fasting does support the body’s counter-regulatory hormone responses and prevents dehydration from worsening hypoglycemia symptoms. If blood sugar drops during a fast, only fast-acting carbohydrates — glucose tablets, juice, or sugar — will raise it effectively.
What happens to blood sugar during Ramadan fasting for diabetics?
Ramadan fasting creates significant challenges for people with diabetes — particularly those on insulin or sulfonylureas — because it involves 12–17 hours of complete food and fluid abstinence. Research shows that without medication adjustment, hypoglycemia risk during Ramadan is substantially elevated. The American Diabetes Association and international diabetes organizations recommend pre-Ramadan medical consultations, dose adjustments, structured blood sugar monitoring, and clear hypoglycemia action plans for all diabetics who intend to fast. Breaking the fast immediately at blood sugar below 70 mg/dL is universally recommended in clinical guidelines.
Conclusion
The answer is clear: yes, fasting can cause low blood sugar — but whether it will cause it for you depends heavily on your health status, medications, and the type of fast you’re doing.
For healthy adults without diabetes or hormonal conditions, standard intermittent fasting carries a very low risk of dangerous hypoglycemia. Your body has sophisticated, multi-layered systems designed specifically to keep blood sugar stable during food deprivation. Those systems generally work well for fasts up to 24 hours and beyond.
But for people on insulin, sulfonylureas, or with conditions affecting cortisol or liver function — fasting without medical preparation and medication adjustment can cause genuine, serious hypoglycemia. The risk is real and the consequences can be severe.
The message is simple: know your risk, talk to your doctor before starting any fasting protocol, monitor your blood sugar during fasting, carry glucose tablets as an emergency tool, and never push through symptoms of hypoglycemia hoping they’ll pass on their own.
Fasting can be a powerful tool for weight loss, metabolic health, and spiritual practice — but it needs to be done with awareness, not ignorance.
This article is for informational purposes only and does not replace personalized medical advice. Always consult your doctor or diabetes care team before beginning any fasting protocol, especially if you take medications that affect blood sugar.
TheAmerican Diabetes Association (ADA) provides comprehensive, regularly updated clinical guidance on hypoglycemia — including its causes, treatment protocols, and specific recommendations for people with diabetes who wish to fast safely.

David Miller: I am a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. I creates clear, practical content to help readers make better everyday health choices. I write evidence-based articles about diabetes, diet, and healthy living. My goal is to simplify complex health topics using trusted sources like WHO and medical journals.