Blood Sugar Monitor Without Finger Pricks: Finally, a Pain-Free Way to Track Your Glucose
If you have diabetes, you know the drill. Multiple finger pricks every single day. Sore fingertips. Blood on your clothes. The constant interruption of your day just to know a number your body should be managing on its own.
It’s exhausting — and for many people, the pain and inconvenience of traditional glucose monitoring is one of the biggest reasons they don’t test as often as they should. But what if you didn’t have to do it that way anymore?
A blood sugar monitor without finger pricks is no longer science fiction. Today, millions of people around the world are tracking their glucose continuously, painlessly, and accurately — using technology that sits quietly on their arm or abdomen and sends real-time readings straight to their phone.
This guide covers everything you need to know: how these devices work, the best options available in 2026, who should use them, how accurate they are, and how to get one. No complicated medical jargon — just clear, honest answers.
Also know about Glucose Tablets for Low Blood Sugar.
What Is a Blood Sugar Monitor Without Finger Pricks?
A blood sugar monitor without finger pricks is a device that measures your glucose levels without needing to draw blood from your fingertip every time you want a reading. The most common type is called a Continuous Glucose Monitor (CGM).
Instead of pricking your finger, a CGM uses a tiny sensor — about the size of a coin — that sits just under your skin (typically on the back of the upper arm or abdomen). This sensor measures glucose levels in the interstitial fluid (the fluid between your cells) rather than directly in your blood. It then transmits readings wirelessly to a smartphone app, a dedicated reader, or an insulin pump every few minutes — around the clock.
This means instead of getting one snapshot reading several times a day, you get a continuous stream of data — showing not just where your blood sugar is right now, but which direction it’s heading and how fast it’s changing.
How Is This Different From a Traditional Glucometer?
| Feature | Traditional Glucometer | CGM (No Finger Prick) |
| Reading frequency | Manual, 4–8 times/day | Every 1–5 minutes, automatically |
| Blood sample needed | Yes — fingertip prick | No (sensor under skin) |
| Real-time trend data | No | Yes — arrows show direction |
| Alerts for highs/lows | No | Yes — automatic alarms |
| Data sharing | No | Yes — with family or doctor |
| Sensor lifespan | N/A (strips only) | 7–15 days per sensor |
| Calibration needed | No | Some require an occasional finger prick |
The difference is significant. A blood sugar monitor without finger pricks gives you far more information with far less effort — and that translates directly into better glucose control.
How Does a CGM Actually Work?
Understanding the technology helps you trust it — and use it better.
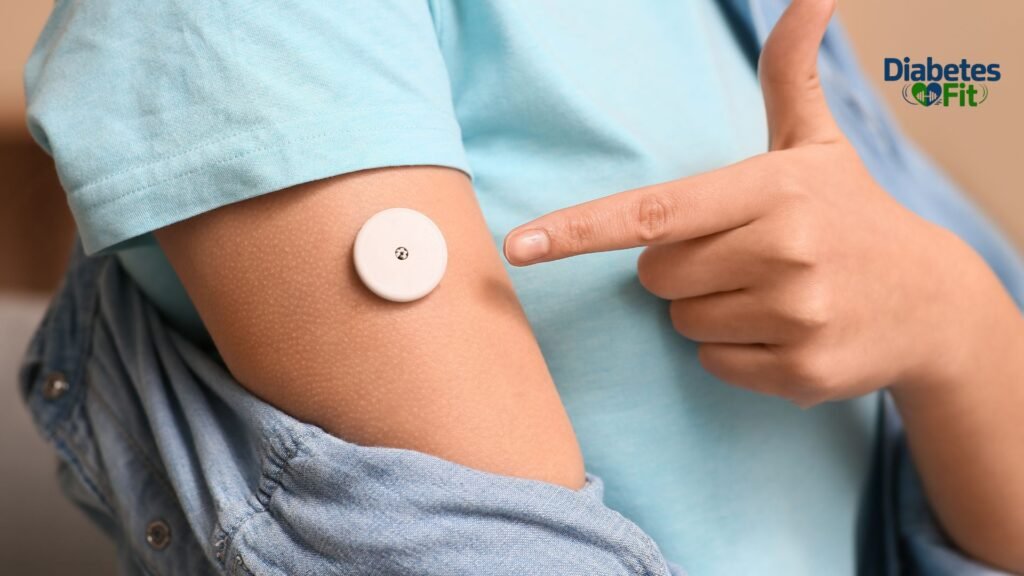
The Sensor
A CGM sensor contains a tiny, flexible filament (thinner than a human hair) that is inserted just below the skin surface using a small applicator. The insertion feels like a small pinch — most people describe it as less painful than a finger prick. Once in place, the sensor is completely flat against the skin and stays in position for 7–15 days, depending on the device.
The sensor continuously measures glucose in the interstitial fluid. Because interstitial glucose closely mirrors blood glucose — with a small lag of about 5–10 minutes — CGM readings are medically accurate for most daily management decisions.
The Transmitter
Attached to the sensor is a small transmitter that wirelessly sends glucose data (usually via Bluetooth) to a receiver, smartphone, smartwatch, or insulin pump every 1–5 minutes.
The Display
You see your glucose reading on your phone screen or device display, along with a trend arrow — one of the most powerful features of CGM technology:
- ↑↑ Rapidly rising
- ↑ Slowly rising
- → Stable
- ↓ Slowly falling
- ↓↓ Rapidly falling
These arrows tell you what your glucose is doing, not just what it is. If you see 90 mg/dL with an ↓↓ arrow, you know you need to act — even though 90 is technically a normal reading.
The Best Blood Sugar Monitors Without Finger Pricks in 2026
Here are the most trusted, widely available CGM devices currently on the market:
1. Dexcom G7
The Dexcom G7 is one of the most popular and highly rated CGM devices available. It’s 60% smaller than its predecessor, the G6, and integrates directly with smartphones and Apple Watch.
Key features:
- Wear time: 10 days per sensor
- Warm-up time: 30 minutes (fastest in its class)
- Accuracy: MARD of 8.2% (very high accuracy)
- No calibration required
- Real-time alerts for highs, lows, and rapid changes
- Compatible with most insulin pumps for closed-loop systems
Best for: People with type 1 or type 2 diabetes who want the most feature-rich experience.
2. Abbott FreeStyle Libre 3
The FreeStyle Libre 3 is a major upgrade from the original Libre. It’s the world’s smallest and thinnest CGM sensor — about the size of two stacked pennies — and it now streams glucose readings automatically every minute without needing to scan.
Key features:
- Wear time: 14 days per sensor
- Automatic readings every minute (no scanning needed)
- Real-time high and low alerts
- Accuracy: MARD of 7.9%
- No calibration required
- Affordable compared to Dexcom
Best for: People who want long sensor wear time, affordability, and a discreet, low-profile device.
3. Medtronic Guardian 4
Designed specifically to integrate with Medtronic’s advanced insulin pump systems for automated insulin delivery (the “artificial pancreas” system).
Key features:
- Wear time: 7 days
- No fingerstick calibration required
- Works with the Medtronic MiniMed 780G pump
- Predictive alerts — warn you before your blood sugar goes high or low
- Excellent integration for pump users
Best for: Type 1 diabetics using Medtronic insulin pumps.
4. Dexcom Stelo (OTC — No Prescription Needed)
Launched in 2024, the Dexcom Stelo was the first CGM approved for over-the-counter sale in the US — no prescription required. This was a landmark development in accessible glucose monitoring.
Key features:
- Wear time: 15 days (longest available)
- No prescription needed
- Designed for type 2 diabetics not on insulin and non-diabetic health-conscious users
- Automatic readings every 5 minutes
- App-based with trend data and insights
Best for: Type 2 diabetics not on insulin, prediabetics, and people who want glucose data for general health and wellness monitoring.
5. Abbott Lingo
Also launched for OTC sale in 2024, the Abbott Lingo CGM is designed for non-diabetic users interested in metabolic health, weight management, and optimizing energy levels through real-time glucose data.
Key features:
- Wear time: 14 days
- No prescription required
- Focused on lifestyle optimization, not just diabetes management
- Pairs with the Lingo app for personalized food and activity insights
Best for: Health-conscious individuals, people with prediabetes, and anyone curious about how their body responds to food and exercise.
Quick Comparison Table
| Device | Wear Time | Prescription Needed | Auto Alerts | Best For |
| Dexcom G7 | 10 days | Yes | Yes | Type 1 & 2 diabetes |
| FreeStyle Libre 3 | 14 days | Yes | Yes | All diabetics |
| Medtronic Guardian 4 | 7 days | Yes | Yes | Pump users |
| Dexcom Stelo | 15 days | No | Yes | Type 2, non-insulin users |
| Abbott Lingo | 14 days | No | Limited | Wellness & prediabetes |
Who Should Use a Blood Sugar Monitor Without Finger Pricks?
CGM technology is no longer just for people with type 1 diabetes. It’s now widely recommended across a broad spectrum of people.
People With Type 1 Diabetes
This group benefits most dramatically. Type 1 diabetes requires constant glucose vigilance — especially around meals, exercise, and sleep. CGM dramatically reduces hypoglycemia risk and improves HbA1c levels by giving continuous data and automatic alerts. Studies show that CGM use in type 1 diabetes reduces hypoglycemic episodes by up to 40%.
People With Type 2 Diabetes on Insulin
For type 2 diabetics managing their condition with insulin, a blood sugar monitor without finger pricks provides the same life-changing benefits as for type 1 — better control, fewer lows, and real-time trend data that guides dosing decisions.
People With Type 2 Diabetes Not on Insulin
Even without insulin, CGM data is enormously valuable. Seeing in real time how specific foods, stress, exercise, and sleep affect blood sugar motivates behavioral change in a way that quarterly HbA1c numbers never can.
People With Prediabetes
CGM can help people with prediabetes understand which foods spike their glucose, motivating dietary and lifestyle changes that may prevent progression to type 2 diabetes.
Pregnant Women With Gestational Diabetes
Glucose control during pregnancy is critical for both mother and baby. CGM provides around-the-clock monitoring that reduces the risk of both hypoglycemia and hyperglycemia during this vulnerable period.
Health-Conscious Non-Diabetics
An emerging group of users — athletes, biohackers, and people focused on metabolic health — are using OTC CGM devices to optimize their diet, energy, and performance based on real glucose data.
How Accurate Is a Blood Sugar Monitor Without Finger Pricks?
Accuracy is the most common concern people have about CGM devices — and it’s a fair one.
CGM accuracy is measured by Mean Absolute Relative Difference (MARD). The lower the MARD percentage, the more accurate the device.
| Device | MARD Score | Accuracy Level |
| FreeStyle Libre 3 | 7.9% | Excellent |
| Dexcom G7 | 8.2% | Excellent |
| Medtronic Guardian 4 | 8.8% | Very Good |
| Dexcom Stelo | ~8.7% | Very Good |
For reference, traditional fingerstick glucometers are considered accurate if their MARD is below 15%. Current CGM devices are as accurate or more accurate than many traditional glucometers for the vast majority of readings.
When CGM Readings May Be Less Accurate:
- During rapid glucose changes, the 5–10 minute lag means CGM may be slightly behind during a fast rise or fall
- Immediately after insertion — during the warm-up period (15–60 minutes)
- When compression occurs, lying on the sensor during sleep can cause temporary false low readings
- During illness with ketoacidosis, some sensors can be affected by elevated ketone levels
For most day-to-day diabetes management, CGM is more than accurate enough. However, if you’re about to make a critical dosing decision — especially with insulin — and your CGM reading doesn’t match how you feel, a confirmatory finger prick is always a safe option.
Cost and Insurance Coverage
One of the most common barriers to using a blood sugar monitor without finger pricks is cost.
Typical Costs (Without Insurance)
| Device | Starter Kit Cost | Monthly Sensor Cost |
| Dexcom G7 | ~$350–$400 | ~$250–$350 |
| FreeStyle Libre 3 | ~$75–$100 | ~$130–$180 |
| Medtronic Guardian 4 | ~$200–$300 | ~$250–$350 |
| Dexcom Stelo (OTC) | ~$99 (2 sensors) | ~$99 for 2 sensors |
| Abbott Lingo (OTC) | ~$49–$79/month | Subscription-based |
Insurance Coverage
- Medicare covers CGM for people with diabetes who use insulin (type 1 and type 2)
- Medicaid coverage varies by state, but is expanding
- Most private insurance plans cover CGM for type 1 diabetics and increasingly for type 2 diabetics on insulin
- Manufacturer savings programs — Dexcom and Abbott both offer savings cards and patient assistance programs for uninsured or underinsured patients
If cost is a concern, ask your doctor specifically about FreeStyle Libre 3 — it’s generally the most affordable prescription CGM option and is widely covered by insurance.
Tips for Getting the Most Out of Your CGM
Once you have a blood sugar monitor without finger pricks, these tips help you use it as effectively as possible:

- Wear it consistently — The power of CGM is in patterns over time. Wearing it only occasionally limits its value.
- Set alerts thoughtfully — Too many alarms cause alert fatigue. Start with alerts at 70 mg/dL (low) and 250 mg/dL (high), then adjust based on your patterns.
- Use trend arrows — Don’t just react to the number; use the arrow to anticipate where glucose is heading.
- Review your AGP report — The Ambulatory Glucose Profile is a summary report generated from your CGM data. Review it with your doctor every 3 months.
- Note meals, exercise, and stress — Many CGM apps let you log these events. Seeing how specific triggers affect your glucose is invaluable.
- Rotate sensor sites — Avoid placing sensors in the same exact spot every time to prevent skin irritation.
- Keep your phone charged — If your phone dies, you lose your readings. A portable charger is a worthwhile investment.
Frequently Asked Questions
Is a CGM completely pain-free?
Almost completely. Inserting the sensor involves a tiny applicator that places a hair-thin filament just below the skin — most people describe it as a small pinch that lasts less than a second. After insertion, the sensor sits flat on the skin and is not felt at all during normal wear. The ongoing experience is genuinely pain-free, which is a significant quality-of-life improvement over multiple daily finger pricks.
Do I still need to do finger pricks if I use a CGM?
Most modern CGMs — including Dexcom G7 and FreeStyle Libre 3 — do not require routine finger-prick calibration. However, your doctor may recommend a confirmatory finger prick if your CGM reading doesn’t match your symptoms, or before making a critical insulin dosing decision. For most daily management, a blood sugar monitor without finger pricks provides sufficient accuracy on its own.
Can I shower, swim, or exercise with a CGM?
Yes. All major CGM devices are waterproof (typically rated IP27 or IP28) and designed to stay in place during showering, swimming, and exercise. The sensor adhesive is designed to hold securely for the full wear period — 7 to 15 days — through normal daily activities, including sweating and water exposure.
Can non-diabetics use a CGM?
Yes — and this is a growing trend. OTC devices like the Dexcom Stelo and Abbott Lingo are specifically designed for non-diabetic users interested in metabolic health. Athletes use CGM to optimize fueling and recovery. People trying to lose weight use it to understand how different foods affect their glucose and hunger levels. You don’t need a diabetes diagnosis to benefit from glucose data.
How long does one CGM sensor last?
Sensor wear time varies by device: Dexcom G7 lasts 10 days, FreeStyle Libre 3 lasts 14 days, Dexcom Stelo lasts 15 days, and Medtronic Guardian 4 lasts 7 days. After the sensor expires, you replace it with a new one. Replacement is quick and easy — most people can apply a new sensor in under 2 minutes.
Is CGM covered by insurance for type 2 diabetes?
Coverage depends on your specific plan and country. In the United States, Medicare covers CGM for type 2 diabetics who use insulin. Many private insurance plans also cover it for insulin-using type 2 diabetics, and coverage is gradually expanding to non-insulin type 2 patients as well. Contact your insurance provider and ask specifically about coverage for “therapeutic CGM” — and have your doctor document medical necessity in their referral.
How does a CGM compare to a traditional glucometer for accuracy?
Modern CGMs are highly accurate — with MARD scores of 7.9%–8.8%, which is comparable to or better than many traditional glucometers (which must be under 15% MARD to receive FDA approval). The main difference is the 5–10 minute lag time in interstitial glucose compared to blood glucose. For routine monitoring and trend analysis, CGM is as reliable as finger-stick testing — and far more informative.
Conclusion
Living with diabetes is hard enough. Painful, inconvenient finger pricks multiple times a day shouldn’t have to be part of the daily routine — not when better technology exists.
A blood sugar monitor without finger pricks gives you more information, more comfort, more safety, and ultimately more freedom. Whether you choose the Dexcom G7 for its cutting-edge features, the FreeStyle Libre 3 for its affordability and long wear time, or the Dexcom Stelo for easy OTC access, you’re choosing a smarter, kinder way to manage your health.
The data these devices provide — continuous, real-time, trend-aware — doesn’t just replace finger pricks. It transforms how you understand your own body. You stop reacting to blood sugar problems after they happen and start anticipating and preventing them before they do.
If you’ve been putting off trying CGM because of cost, confusion, or habit, talk to your doctor at your next appointment. Ask specifically about a blood sugar monitor without finger pricks. The conversation could genuinely change your life.
If this guide helped you understand CGM better, share it with someone who’s still pricking their fingers ten times a day. They deserve to know this option exists.
This article is for informational purposes only and does not replace personalized medical advice. Always consult your doctor or diabetes care team before switching or starting any new glucose monitoring device.
TheU.S. Food and Drug Administration (FDA) maintains an official, up-to-date page on approved continuous glucose monitoring devices — including safety information, cleared devices, and guidance for patients and caregivers.

David Miller: I am a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. I creates clear, practical content to help readers make better everyday health choices. I write evidence-based articles about diabetes, diet, and healthy living. My goal is to simplify complex health topics using trusted sources like WHO and medical journals.







