Continuous Glucose Monitor (CGM): How It Works and Is It Worth It in 2026? Everything You Need to Know Before You Buy
Blood sugar management has entered a new era — and the Continuous Glucose Monitor is at the center of it. Whether you have Type 1 diabetes, Type 2 diabetes, prediabetes, or simply want to understand how your body responds to food and stress in real time, the question everyone is asking in 2026 is the same: Is a Continuous Glucose Monitor actually worth it?
Also know about the Best Store-Bought Chips for Diabetics in the USA.
CGM technology has advanced dramatically, prices have dropped, over-the-counter options now exist, and millions of people without diabetes are strapping these devices to their arms for metabolic insight. But with so many choices and so much marketing noise, cutting through to the honest answer matters. In this guide, you will learn precisely how a Continuous Glucose Monitor works, which devices lead the market in 2026, who genuinely benefits, what it realistically costs, and whether the investment makes sense for your specific situation.
What Exactly Is a Continuous Glucose Monitor?
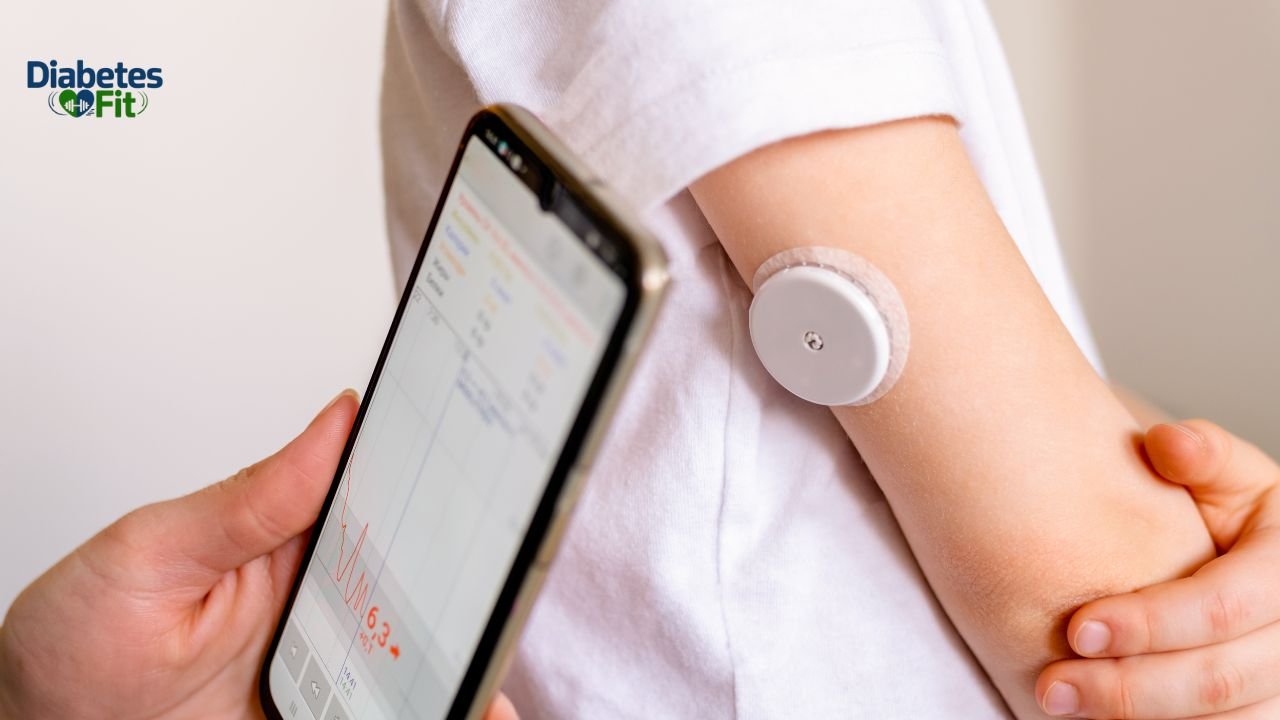
A Continuous Glucose Monitor — commonly shortened to CGM — is a small wearable device that measures your glucose levels continuously throughout the day and night, automatically, without requiring you to prick your finger each time you want a reading.
Instead of giving you one isolated glucose snapshot like a traditional glucometer, a Continuous Glucose Monitor delivers a complete, ongoing picture of your blood sugar — showing you not just where your glucose is right now, but where it has been for the past several hours, which direction it is currently moving, and how fast that movement is happening.
In practical terms, imagine the difference between checking the weather once a day versus watching a live weather radar. One gives you a single data point. The other gives you the full picture — patterns, trends, and early warnings before a storm arrives.
That is exactly what a CGM does for blood sugar management.
How Does a Continuous Glucose Monitor Actually Work?
Understanding the technology behind a Continuous Glucose Monitor removes the mystery and helps you use it more effectively. The system has three connected parts that work together continuously.
Part One: The Sensor Beneath Your Skin
The sensor is the foundation of every CGM system. It is a tiny, flexible filament — thinner than a human hair and typically between 4 and 7 millimeters long — that is inserted just beneath the skin using a small spring-loaded applicator. Most people describe the insertion as a brief pinch that is equal to or less uncomfortable than a standard finger prick.
The sensor typically sits on the back of the upper arm or on the abdomen. Once inserted, it rests in the interstitial fluid — the thin layer of fluid that bathes the cells just beneath your skin.
Here is the chemistry that makes everything work. The sensor filament is coated with an enzyme called glucose oxidase. When glucose molecules from the interstitial fluid come into contact with this enzyme, a precise chemical reaction occurs that generates a tiny electrical current. The strength of that electrical current is directly proportional to the concentration of glucose present — more glucose, stronger current. The sensor measures this current continuously and converts it into glucose readings.
One important detail to understand: the Continuous Glucose Monitor measures glucose in interstitial fluid, not directly in the blood. Glucose moves from the bloodstream into interstitial fluid with a physiological delay of approximately 5 to 15 minutes. This means that during periods of rapidly changing blood sugar — immediately after eating or during intense exercise — CGM readings can briefly lag behind actual blood glucose levels. Modern devices use sophisticated predictive algorithms to account for this lag and provide accurate trend data despite it.
Part Two: The Transmitter That Sends the Data
The transmitter is attached to the sensor on the skin. In all current 2026 CGM systems, the transmitter and sensor have been integrated into a single compact unit — typically a small disc or oval device secured to the skin with medical-grade adhesive. The entire on-skin profile is slim enough that it sits almost flat against your arm or abdomen.
The transmitter’s job is straightforward but critical: receive the electrical glucose signal from the sensor and wirelessly transmit the reading to your display device. Modern CGM transmitters communicate via Bluetooth, sending a new glucose reading every 1 to 5 minutes, depending on the specific device. Many current systems also incorporate near-field communication (NFC), allowing you to get a reading simply by holding your phone near the sensor — no Bluetooth pairing required.
Battery life in 2026 transmitters has improved considerably. Many are now fully integrated into the disposable sensor unit and do not require separate charging or replacement.
Part Three: The App That Displays Your Data
The display component is where your glucose data becomes actionable. In virtually all CGM systems available in 2026, the primary display is a dedicated smartphone app available for both iOS and Android.
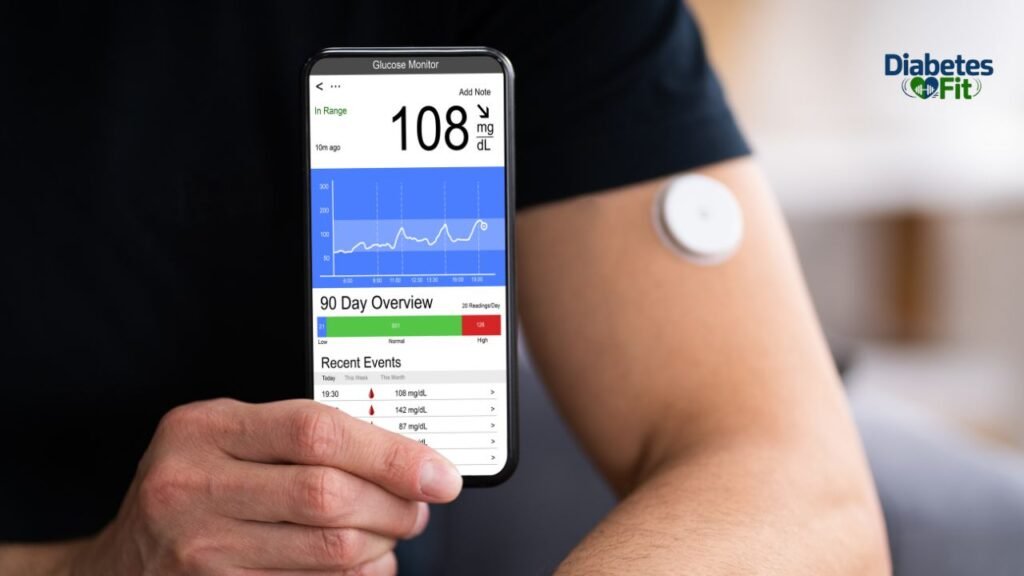
The app shows you far more than a simple number. A typical Continuous Glucose Monitor app interface includes:
- Your current glucose reading in real time
- A trend arrow showing the direction and rate of glucose change
- A continuous graph of your glucose levels over the past 1, 3, 6, or 24 hours
- Color-coded alerts when glucose moves above or below your customized targets
- Summary statistics including time in range, time above range, and time below range
- Pattern recognition showing how your glucose behaves at specific times of day or after certain meals
- In many systems, integration with food logging, exercise tracking apps, and smartwatches
The trend arrow deserves special mention because it is one of the most clinically valuable features a CGM provides. Knowing that your glucose is currently 120 mg/dL means one thing when the arrow points steadily horizontal. It means something entirely different — and requires a different response — when the arrow points sharply downward, indicating a rapid drop. A traditional glucometer can never tell you that.
CGM vs. Traditional Glucometer: Why the Difference Matters
For people who have been managing diabetes with a standard glucometer for years, understanding what a Continuous Glucose Monitor adds to the picture is important before deciding whether the upgrade is worthwhile.
| Feature | Traditional Glucometer | Continuous Glucose Monitor |
| Readings per day | 2 to 8 (manual) | 288 to 1,440 (automatic) |
| Requires finger prick | Every single reading | Rarely or never |
| Shows trend direction | Never | Always |
| Overnight monitoring | Not practical | Complete and automatic |
| Customizable alerts | None | Fully customizable |
| Detects nocturnal lows | Cannot | Yes — wakes you with an alarm |
| Pattern analysis | Minimal | Comprehensive |
| Data sharing capability | None | Real-time to caregivers |
| Monthly cost estimate | $10 to $35 | $75 to $350 |
| Insulin pump integration | No | Yes (select devices) |
The critical gap that a glucometer cannot fill is the invisible hours — every moment between manual tests. If your blood sugar drops dangerously low at 3 AM, a glucometer cannot warn you. A Continuous Glucose Monitor can.
Who Genuinely Benefits from a CGM in 2026?
The appropriate user base for a Continuous Glucose Monitor has expanded significantly over the past few years. Here is an honest breakdown by category.
Type 1 Diabetes — The Clearest Case
For people living with Type 1 diabetes, a Continuous Glucose Monitor is no longer an optional upgrade — it has become the clinical standard of care in 2026. The evidence is simply too strong to ignore.
Multiple landmark clinical trials have demonstrated that CGM use in Type 1 diabetes:
- Significantly reduces HbA1c — the primary long-term blood sugar marker
- Reduces time spent in hypoglycemia by 30 to 40%
- Increases time in range — the percentage of each day spent with blood sugar in the healthy target zone
- Dramatically reduces the frequency and severity of nocturnal hypoglycemia
- Improves quality of life and reduces diabetes-related distress
When combined with an insulin pump in a closed-loop system — sometimes called an artificial pancreas — the Continuous Glucose Monitor becomes the sensory input that allows the system to automatically adjust insulin delivery every few minutes based on real-time glucose data. This technology represents the most significant advance in Type 1 diabetes management in decades, and it is entirely dependent on CGM as its foundation.
Type 2 Diabetes on Insulin
For Type 2 diabetics using insulin, the safety case for CGM mirrors that of Type 1. Hypoglycemia — particularly silent nocturnal hypoglycemia — carries the same cardiovascular and neurological risks regardless of diabetes type. Detecting low glucose events that would otherwise go completely unnoticed is a potentially life-saving capability.
Beyond safety, research published in JAMA Internal Medicine found that CGM use in non-intensively managed Type 2 diabetes produced meaningful HbA1c reductions even without insulin dose adjustments — suggesting that the behavioral feedback from seeing real-time glucose data alone drives better self-management decisions.
Type 2 Diabetes Managed Without Insulin
This is a growing and genuinely valuable use case. Seeing exactly how a bowl of white rice, a slice of sourdough bread, or a piece of fruit affects your personal blood glucose in real time is far more motivating and behaviorally effective than reading a general glycemic index chart.
Personalized CGM-guided nutrition coaching has emerged as an evidence-backed approach for improving glycemic control in non-insulin Type 2 diabetes. Studies show that when people use CGM data to understand their individual food responses and modify their eating patterns accordingly, they achieve glucose improvements comparable to adding a second medication — without the medication.
Prediabetes
Approximately 98 million American adults had prediabetes in 2026. The vast majority are unaware of it. A short-term CGM trial for someone with a prediabetes diagnosis provides critical personalized information: which foods spike your glucose most severely, how well your body recovers after meals, and whether your fasting glucose is showing worrying patterns.
This information motivates change in a way that abstract warnings about future diabetes risk simply do not. Seeing your own glucose spike to 185 mg/dL after eating a bagel is viscerally different from being told your HbA1c is 5.9. One is a number on a lab report. The other is your body in action.
Health-Conscious Non-Diabetics
The most controversial — and fastest-growing — CGM user group is metabolically healthy people with no diabetes diagnosis. Athletes using CGM to optimize pre-workout nutrition and race-day fueling, executives monitoring how stress and poor sleep affect their metabolic health, and weight loss seekers using CGM to identify hidden dietary glucose triggers all fall into this category.
The clinical evidence for CGM benefits in truly healthy people is still accumulating. What is clear is that many users in this group report meaningful behavioral changes and improved metabolic awareness — and the arrival of affordable, over-the-counter CGM options in 2026 has made this accessible for the first time without a prescription.
Top CGM Devices in 2026: Ranked and Compared
Dexcom G7 — Best Clinical Performance
The Dexcom G7 remains the benchmark for clinical accuracy and comprehensive feature integration in 2026.
Key facts:
- Sensor wear: 10 days per sensor
- Accuracy: approximately 8.2% MARD — excellent clinical grade
- Warm-up time: just 30 minutes after insertion
- Integration: compatible with leading insulin pumps for closed-loop systems
- Alerts: fully customizable high, low, and urgent low alarms
- Data sharing: real-time glucose sharing with up to 10 followers via app
- Smartwatch support: Apple Watch and select Android Wear devices
- Prescription required: Yes
Best for: Type 1 diabetes, insulin pump users, and anyone requiring the highest clinical accuracy.
Abbott FreeStyle Libre 3 — Best Accuracy-to-Value Ratio
The FreeStyle Libre 3 has cemented its position as the most widely used CGM globally — and for very good reasons.
Key facts:
- Sensor wear: 14 days — longest clinical sensor on the market
- Accuracy: approximately 7.9% MARD — marginally the most accurate major CGM
- Sensor size: the smallest available — barely larger than a large coin
- Automatic Bluetooth streaming: real-time, continuous readings to the smartphone
- Alerts: high and low alarm system
- Cost: generally the most affordable prescription CGM with broad insurance coverage
- Prescription required: Yes for Libre 3; Libre 2 Plus available OTC
Best for: Type 1, Type 2, prediabetes, first-time CGM users, cost-sensitive users.
Dexcom Stelo — Best Over-the-Counter Option
The Stelo is Dexcom’s purpose-built CGM for the non-prescription wellness and metabolic health market.
Key facts:
- Sensor wear: 15 days — the longest single sensor duration available
- No prescription required — available directly from Dexcom’s website and select pharmacies
- Designed for adults without diabetes or those with non-insulin-managed diabetes
- No emergency low alerts (designed for trend monitoring, not critical alerting)
- App includes meal logging and personalized glucose insights
- Monthly cost without insurance: approximately $89 to $99
Best for: Non-diabetics, prediabetics, health optimizers, people who want metabolic data without visiting a doctor.
Abbott Lingo — Best for Guided Wellness Coaching
Abbott’s Lingo targets the same non-prescription wellness market as the Stelo, with a strong emphasis on AI-powered coaching and behavioral guidance.
Key facts:
- Sensor wear: 14 days
- No prescription required
- AI coaching engine interprets glucose patterns and provides personalized dietary and lifestyle recommendations
- Subscription model with coaching features integrated directly in the app
- Monthly cost: approximately $49 to $89, depending on subscription tier
Best for: Non-diabetics who want guided interpretation of their CGM data, people focused on weight management, and energy optimization.
Medtronic Guardian 4 — Best for Medtronic Pump Users
The Guardian 4 is built specifically for seamless integration with Medtronic’s insulin pump platform.
Key facts:
- Sensor wear: 7 days
- No fingerstick calibration required
- Designed exclusively for closed-loop use with Medtronic MiniMed insulin pumps
- Less relevant as a standalone CGM
Best for: Existing Medtronic pump users seeking full closed-loop integration.
2026 CGM Device Summary Table
| Device | Wear Duration | Prescription | Accuracy MARD | OTC | Ideal User | Monthly Cost |
| Dexcom G7 | 10 days | Yes | ~8.2% | No | Type 1, pump users | $120–180 insured |
| FreeStyle Libre 3 | 14 days | Yes | ~7.9% | Libre 2 Plus only | Type 1, Type 2, budget | $75–130 insured |
| Dexcom Stelo | 15 days | No | Good | Yes | Non-diabetic, prediabetes | $89–99 |
| Abbott Lingo | 14 days | No | Good | Yes | Wellness, coaching | $49–89 |
| Medtronic Guardian 4 | 7 days | Yes | Excellent | No | Medtronic pump users | $150–200 insured |
What Does a CGM Cost in 2026? Insurance, OTC, and Out-of-Pocket
Cost is one of the most important practical factors in the CGM decision. Here is the 2026 landscape:
Insurance Coverage in the USA
Coverage has expanded meaningfully in recent years:
- Medicare Part B: Covers CGM for all insulin-treated diabetics. A 2024 expansion also opened coverage for non-insulin Type 2 diabetics with documented hypoglycemia risk.
- Medicaid: Coverage varies by state, but most states cover CGM for Type 1 and insulin-using Type 2 diabetics.
- Private insurance: Most major commercial plans cover CGM for Type 1 diabetes. Type 2 coverage depends on insulin use and specific plan terms. Always check your formulary.
- HSA and FSA eligible: All major CGM systems qualify as HSA and FSA eligible medical expenses in 2026.
Out-of-Pocket Costs Without Insurance
| Scenario | Estimated Monthly Cost |
| Dexcom G7 (no insurance) | $250–350 |
| FreeStyle Libre 3 (no insurance) | $150–220 |
| Stelo (OTC, no prescription needed) | $89–99 |
| Lingo (OTC subscription) | $49–89 |
| Traditional glucometer comparison | $15–35 |
Is a Continuous Glucose Monitor Worth It in 2026? The Verdict
Let us deliver the direct, differentiated verdict:
If you have Type 1 diabetes, A CGM is absolutely worth it. Full stop. The clinical evidence is definitive, insurance coverage is broad, and the safety and quality-of-life benefits are transformative.
If you have Type 2 diabetes on insulin: A CGM is worth it. The hypoglycemia detection benefit alone justifies the cost, and insurance coverage has improved substantially.
If you have Type 2 diabetes managed without insulin: A CGM is worth it for a defined educational period of 1 to 3 months. The personalized dietary insights you gain will inform your food choices for years and may produce glucose improvements equivalent to adding a medication.
If you have prediabetes: A short CGM trial is worth it. The behavioral impact of seeing your own real-time glucose responses to food is far more motivating than generic dietary advice alone.
If you are metabolically healthy but curious: The OTC options at $49 to $99 per month make a 1 to 2 month trial reasonable if you have specific goals — optimizing athletic performance, understanding energy crashes, or identifying hidden dietary triggers. For casual curiosity without defined goals, the cost-benefit ratio is less compelling.
Frequently Asked Questions
How painful is CGM sensor insertion?
Sensor insertion is far less uncomfortable than most people anticipate. The spring-loaded applicator inserts the tiny filament quickly — most users describe it as a brief pinch at most, often less noticeable than a traditional finger prick. After insertion, the sensor is not painful to wear. The majority of users report forgetting it is there within a few hours. Occasional mild skin irritation from the adhesive occurs in some users, which is typically managed with skin barrier wipes or alternative adhesive patches.
How accurate is a CGM compared to a blood glucose meter?
Modern CGMs are highly accurate for clinical use. The FreeStyle Libre 3 achieves approximately 7.9% MARD, and the Dexcom G7 approximately 8.2% MARD — meaning readings are within roughly 8% of true blood glucose on average. Traditional glucometers are required to meet FDA standards of within 15% accuracy. Discrepancies between CGM and fingerstick readings can occur during rapidly changing glucose levels due to the physiological lag between interstitial and blood glucose. For insulin dosing during rapid changes, confirming with a fingerstick remains the recommended standard practice.
Can you wear a CGM while swimming or exercising?
Yes — all major 2026 CGM sensors are water-resistant and designed for active use. Both the Dexcom G7 and FreeStyle Libre 3 are rated water-resistant to a depth suitable for swimming and showering. The medical-grade adhesive is designed to remain secure through water, sweat, and physical activity for the full sensor wear period. Athletes commonly use additional overlay adhesive patches for high-intensity or prolonged water activities. Exercise typically does not affect sensor accuracy, though the physiological lag may be slightly more pronounced during intense exercise as blood flow distribution changes.
Will a CGM work with my smartwatch?
Many 2026 CGM systems offer smartwatch display integration. The Dexcom G7 displays glucose readings directly on Apple Watch and select Wear OS devices. The FreeStyle Libre 3 similarly supports Apple Watch display through its app. This means your glucose level and trend arrow are visible with a quick glance at your wrist — an especially useful feature for athletes and anyone who wants discreet monitoring without pulling out their phone. Integration capabilities continue to expand as both Apple and Google have deepened health platform integration with CGM manufacturers.
Can children use a Continuous Glucose Monitor?
Yes — CGM is widely used in pediatric diabetes management and is considered standard of care for children with Type 1 diabetes. The Dexcom G7 is FDA-approved for use in children aged 2 years and older. The FreeStyle Libre 3 is approved for children aged 4 and older. The remote data sharing capability is particularly valuable in pediatric use — parents can monitor their child’s glucose levels in real time from a separate phone, receiving alerts for lows or highs even when they are not in the same room. Many school nurses and caregivers also follow shared CGM data to ensure safety during school hours.
What happens when a CGM sensor reaches the end of its wear period?
When a sensor reaches the end of its programmed wear period — 10 days for the Dexcom G7, 14 days for FreeStyle Libre 3 — the app notifies you that the sensor has expired and needs to be replaced. Replacement is simple: remove the expired sensor from your skin, apply a new sensor using the applicator, and start the brief warm-up period before readings resume. Used sensors are disposed of as medical waste according to local regulations. Many users develop a sensor rotation pattern — alternating between the upper arms and occasionally the abdomen — to give skin areas adequate recovery time between applications.
Is CGM data private, and who can see it?
CGM data privacy is an important consideration. All major CGM apps encrypt glucose data and store it on secure cloud servers. You control who has access to your data — sharing is opt-in only. Most apps offer a follower-sharing feature where you can designate specific people, such as a spouse, parent, or caregiver, to view your glucose data in real time through a companion app on their device. Healthcare providers can access data through separate provider portals if you choose to share. CGM manufacturers’ data practices are governed by HIPAA in the USA for prescription devices. Reading the privacy policy of any CGM app is recommended before use, particularly for OTC wellness devices where HIPAA protections may be less comprehensive.
Conclusion
The Continuous Glucose Monitor has transformed from a specialized tool for the most complex diabetes cases into a broadly accessible technology that benefits a wide spectrum of people — from those managing life-threatening blood sugar instability to health-conscious individuals seeking deeper metabolic self-knowledge.
In 2026, a Continuous Glucose Monitor is worth it for virtually anyone whose health is meaningfully affected by blood sugar dynamics. The clinical evidence for its benefits in Type 1 and Type 2 diabetes is definitive and has only strengthened with time. The expansion into prediabetes and metabolic health represents a genuine prevention opportunity at a population scale. And the arrival of prescription-free options like the Stelo and Lingo has removed the final barrier for people who want to understand their metabolic health without a diabetes diagnosis.
A Continuous Glucose Monitor does not change what your body does with food, stress, and sleep. But it makes the invisible visible — and in that visibility lies the power to make genuinely informed decisions about your health every single day. That is what makes a CGM worth it in 2026 and beyond.
If you are considering a CGM and have diabetes, your next step is a conversation with your endocrinologist or primary care physician about which device is covered by your insurance and best suited to your management needs. If you are non-diabetic and want to start today, the Stelo and Lingo are available without a prescription and can be ordered online right now.
Your blood sugar has a story to tell. A CGM helps you finally hear it.
Medical Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. All CGM-related decisions for diabetes management should be made in consultation with a qualified healthcare provider. Individual device availability, pricing, and insurance coverage may vary.
Also, read more from Cleveland Clinic.

David Miller: I am a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. I creates clear, practical content to help readers make better everyday health choices. I write evidence-based articles about diabetes, diet, and healthy living. My goal is to simplify complex health topics using trusted sources like WHO and medical journals.