Insulin Resistance Symptoms and Treatment Options You Need to Know Before It’s Too Late
What Is Insulin Resistance — And Why Should You Care?
Millions of people are walking around right now with insulin resistance symptoms and have absolutely no idea. No obvious warning label. No flashing alarm. Just silent damage building up inside the body — until, one day, a doctor delivers the diagnosis of prediabetes or type 2 diabetes.
Understanding insulin resistance symptoms and treatment options you need to know is one of the most important things you can do for your long-term health. Whether you’ve been told your blood sugar is “a little high,” or you’re just feeling tired, gaining weight around your belly, or craving sugar constantly, this article is written for you.
We’ll break down what insulin resistance actually means, what signs to watch for, what causes it, and most importantly — what you can do about it. No medical jargon. Just real, practical information.
Also know about the Continuous Glucose Monitor (CGM).
Understanding Insulin Resistance: The Basics
To understand insulin resistance, you first need to know what insulin does. Insulin is a hormone made by your pancreas. Its job is to act like a key — it opens your body’s cells so glucose (sugar from food) can enter and be used as energy.
When you have insulin resistance, your cells stop responding properly to that key. Imagine trying to open a lock, but the keyhole is partially blocked. Your pancreas works harder and pumps out more insulin to try to get the job done. Over time, the pancreas gets tired. Blood sugar starts to rise. And that’s when the real trouble begins.
Insulin resistance is often called a “silent condition” because it develops slowly, over years, and early symptoms are easy to dismiss or blame on stress or aging.
Top Insulin Resistance Symptoms and Treatment Options You Need to Know
Recognizing insulin resistance symptoms early gives you the best chance to reverse the condition before it turns into something more serious. Here are the most common signs:
1. Constant Fatigue and Brain Fog

Feeling exhausted even after a full night of sleep? When your cells can’t absorb glucose properly, your body doesn’t get the energy it needs. This leads to constant tiredness and difficulty concentrating. Many people describe it as feeling “foggy” or struggling to think clearly after meals.
2. Belly Fat and Weight Gain
Extra weight around the midsection — sometimes called “belly fat” or “visceral fat” — is one of the most visible signs of insulin resistance. When insulin levels are high, the body stores more fat, especially around the abdomen. A waist measurement of more than 35 inches in women or 40 inches in men can be a warning sign.
3. Strong Sugar and Carb Cravings
When cells don’t get enough glucose for energy, your brain sends out urgent hunger signals — especially for sugar and refined carbohydrates. This craving cycle is frustrating and difficult to break without addressing the underlying insulin resistance.
4. High Blood Sugar Levels

A fasting blood glucose above 100 mg/dL is considered prediabetes territory. Many people don’t test regularly and miss this early warning sign. Insulin resistance is one of the primary drivers of elevated blood sugar.
5. Dark Patches on the Skin (Acanthosis Nigricans)
One of the more distinctive insulin resistance symptoms is dark, velvety patches of skin that appear around the neck, armpits, or groin area. This happens because high insulin levels stimulate skin cells to multiply. It’s a physical sign that insulin levels have been elevated for some time.
6. High Triglycerides and Low HDL Cholesterol
Blood tests often reveal this combination in people with insulin resistance. High triglycerides (above 150 mg/dL) and low HDL (good) cholesterol are closely linked to excess insulin in the bloodstream and are part of a condition called metabolic syndrome.
7. Frequent Hunger Shortly After Eating

Feeling hungry again just an hour or two after a full meal is a classic sign. When cells resist insulin, they’re not absorbing nutrients efficiently, leaving you feeling unsatisfied even when you’ve eaten enough.
8. High Blood Pressure
Excess insulin causes the kidneys to retain more sodium, which can raise blood pressure. Studies show a strong link between insulin resistance and hypertension, especially in people who are overweight.
9. Polycystic Ovary Syndrome (PCOS) in Women
PCOS and insulin resistance are deeply connected. In fact, insulin resistance is found in up to 70% of women with PCOS. Symptoms include irregular periods, excess hair growth, acne, and difficulty losing weight.
10. Skin Tags
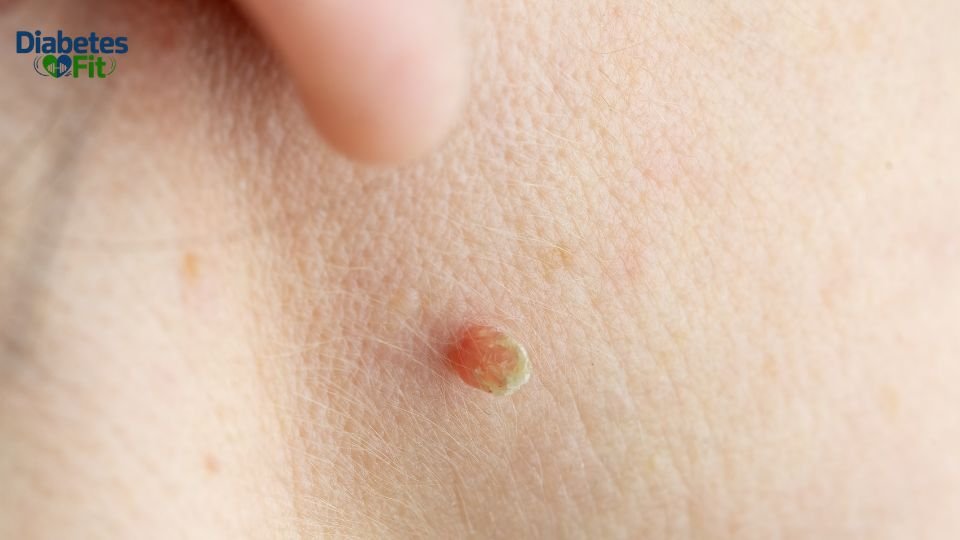
Small, benign growths of skin — especially around the neck or armpits — are often associated with insulin resistance. They’re harmless on their own but can be a useful visual signal that something is off metabolically.
Quick Reference: Insulin Resistance Symptoms at a Glance
| Symptom | What It Means | Severity Level |
| Constant fatigue | Cells not getting enough glucose for energy | Moderate |
| Belly fat | High insulin promoting fat storage | High |
| Sugar cravings | Brain demanding quick glucose fuel | Moderate |
| Dark skin patches | Skin cells reacting to excess insulin | High |
| High triglycerides | Liver overproducing fat due to insulin | High |
| Frequent hunger | Nutrients not absorbed properly | Moderate |
| Brain fog | Unstable glucose affecting brain function | Moderate |
| High blood pressure | Sodium retention from excess insulin | High |
| PCOS symptoms | Hormonal disruption from insulin resistance | High |
| Skin tags | Skin response to chronically high insulin | Low–Moderate |
What Causes Insulin Resistance? Common Risk Factors
Insulin resistance doesn’t happen overnight. It builds up over time, driven by a mix of lifestyle and genetic factors. Understanding the causes can help you take control:

• Poor diet high in refined carbohydrates, sugar, and processed foods
• Physical inactivity and a sedentary lifestyle
• Excess body fat, especially visceral (belly) fat
• Chronic stress and elevated cortisol levels
• Poor sleep or sleep apnea
• Family history of type 2 diabetes
• Age (risk increases after 45, but younger people are not immune)
• Hormonal disorders like Cushing’s syndrome or PCOS
• Certain medications, including steroids and some antipsychotics
One important point: insulin resistance is not your fault. Genetics play a real role. But the encouraging news is that lifestyle changes have an enormous impact — far more than most people realize.
How Is Insulin Resistance Diagnosed?
There is no single test that diagnoses insulin resistance directly. Instead, doctors look at a combination of blood tests and physical signs. Here are the most common diagnostic tools:
| Test | What It Measures | Normal vs. Warning Range |
| Fasting blood glucose | Blood sugar after an overnight fast | Normal: <100 mg/dL | Prediabetes: 100–125 |
| HbA1c | Average blood sugar over 3 months | Normal: <5.7% | Prediabetes: 5.7%–6.4% |
| Fasting insulin level | Insulin in the blood when fasting | Optimal: <10 uIU/mL | High risk: >15 |
| Triglycerides | Blood fat levels | Healthy: <150 mg/dL | High risk: >200 |
| HDL cholesterol | Good cholesterol level | Healthy: >50 mg/dL (women) / >40 (men) |
| HOMA-IR score | Calculated insulin resistance index | Score >2.0 suggests insulin resistance |
If you’re concerned about insulin resistance, ask your doctor to run a fasting insulin test along with your regular blood glucose; many standard panels skip this important marker.
Insulin Resistance Treatment Options You Need to Know
Here is the genuinely good news: insulin resistance is one of the most reversible conditions in medicine. The right changes — made consistently — can restore normal insulin sensitivity and dramatically reduce your risk of type 2 diabetes. Here’s what works:
1. Change Your Diet First
This is the single most powerful tool you have. The goal is to stop flooding your bloodstream with glucose and give insulin levels a chance to come down.
• Reduce refined carbohydrates: white bread, pasta, sugary drinks, pastries
• Eat more fiber: vegetables, legumes, berries, whole grains
• Choose healthy fats: olive oil, avocado, nuts, fatty fish
• Prioritize protein at every meal to slow glucose absorption
• Try a low-glycemic or Mediterranean-style eating plan
• Limit alcohol, which raises triglycerides and disrupts insulin signaling
Studies consistently show that a Mediterranean diet or low-carbohydrate diet can significantly reduce insulin resistance markers within just a few weeks of consistent effort.
2. Exercise Regularly (Even Small Amounts Help)
Physical activity is one of the fastest ways to improve insulin sensitivity. When your muscles contract during exercise, they absorb glucose directly — without needing insulin. This gives your cells a rest and trains them to respond better.
• Aim for at least 150 minutes of moderate exercise per week
• Brisk walking, cycling, and swimming are excellent starting points
• Add strength training 2–3 times a week — muscle tissue uses more glucose
• Even a 15-minute walk after meals significantly lowers post-meal blood sugar
3. Lose Excess Body Weight
Losing just 5–10% of your body weight can lead to meaningful improvements in insulin sensitivity. You don’t need to reach an “ideal” weight — even modest weight loss makes a measurable difference in blood sugar and insulin levels.
4. Improve Your Sleep
Poor sleep directly worsens insulin resistance. A single night of bad sleep can reduce insulin sensitivity by up to 25%. Prioritize 7–9 hours of quality sleep per night. If you snore heavily or wake up tired, get checked for sleep apnea — it’s a strong driver of insulin resistance and often goes undiagnosed.
5. Manage Stress Actively
Chronic stress elevates cortisol, which raises blood sugar and drives fat storage in the belly. Proven stress-reduction strategies include:
• Daily meditation or deep breathing exercises (even 10 minutes helps)
• Regular physical activity (this also reduces stress)
• Spending time outdoors and in nature
• Setting healthy boundaries with work and technology
6. Medications When Needed
In some cases, lifestyle changes alone aren’t enough, and your doctor may recommend medication. The most commonly used medications for insulin resistance include:
| Medication | How It Works | Common Use |
| Metformin | Reduces liver glucose production, improves sensitivity | Prediabetes, type 2 diabetes, PCOS |
| GLP-1 agonists (e.g., semaglutide) | Regulates blood sugar and promotes weight loss | Type 2 diabetes, obesity |
| Thiazolidinediones (TZDs) | Directly improve insulin sensitivity in cells | Type 2 diabetes |
| SGLT2 inhibitors | Causes kidneys to excrete excess glucose | Type 2 diabetes, heart failure |
Always work with your healthcare provider before starting or stopping any medication. These drugs are most effective when combined with lifestyle changes.
7. Consider Targeted Supplements (With Doctor Guidance)
Several supplements have research support for improving insulin sensitivity, though they should complement — not replace — lifestyle changes:
• Berberine: Strong evidence for lowering blood sugar, sometimes compared to metformin
• Magnesium: Deficiency is linked to insulin resistance; supplementing may help
• Inositol (especially myo-inositol): Helpful for PCOS-related insulin resistance
• Alpha-lipoic acid: Antioxidant that may improve insulin signaling
• Chromium: May support blood sugar regulation
Can You Prevent Insulin Resistance?
Yes — and prevention is always better than treatment. Many people who develop insulin resistance could have avoided it with earlier action. Here are the most effective preventive steps:
• Maintain a healthy body weight throughout life
• Stay physically active — even light daily movement matters
• Eat a whole-food, plant-rich diet with minimal processed foods
• Get regular blood sugar checks, especially after age 35
• Know your family history and share it with your doctor
• Prioritize sleep and stress management as health fundamentals
Prevention is particularly important for people with a family history of type 2 diabetes, women with PCOS, and people who are overweight. These groups should be tested more frequently and proactively.
Living With Insulin Resistance: A Day-in-the-Life Guide
Reversing insulin resistance isn’t about perfection — it’s about consistent, sustainable habits. Here’s what a typical day might look like for someone actively managing their insulin resistance:
| Time of Day | Action | Why It Helps |
| Morning | Protein-rich breakfast (eggs, Greek yogurt, nuts) | Slows glucose rise, reduces cravings |
| After breakfast | 10–15 min walk | Lowers post-meal blood sugar directly |
| Midday | Vegetable-heavy lunch, limit white rice/bread | Reduces glycemic load |
| Afternoon | Avoid sugary snacks; choose nuts or cheese | Keeps insulin levels stable |
| Evening | Strength training or brisk walk for 30 min | Boosts insulin sensitivity overnight |
| Dinner | Balanced plate: protein, fat, fiber-rich carbs | Prevents blood sugar spikes |
| Bedtime | Consistent sleep schedule, screen-free wind-down | Improves insulin sensitivity the next day |
Conclusion
Insulin resistance symptoms and treatment options you need to know about are not as complicated as the medical world sometimes makes them seem. At its core, this condition responds beautifully to the basics: move your body, eat real food, sleep well, and manage stress.
The most important step is the first one — awareness. Now that you understand the key insulin resistance symptoms and treatment options, you’re in a far better position than most people who are quietly developing this condition without knowing it.
Whether you’ve just been diagnosed, suspect you have insulin resistance, or simply want to protect your long-term health, the changes that reverse insulin resistance are the same ones that improve every aspect of your wellbeing. You don’t need to do everything at once. Start with one change today. Build from there.
Talk to your doctor about testing your fasting insulin alongside your regular blood work. Ask questions. Be your own health advocate. The earlier you catch and address insulin resistance, the better your chances of reversing it completely — and living a healthier, more energetic life for years to come.
Frequently Asked Questions
What are the first signs of insulin resistance?
The earliest signs are often subtle: unexplained fatigue, increased belly fat, persistent sugar cravings, and feeling hungry shortly after eating. Some people also notice dark patches of skin around the neck or armpits. Because these symptoms are easy to ignore, many people don’t realize they have insulin resistance until a routine blood test reveals elevated blood sugar.
Can insulin resistance be reversed completely?
Yes, for many people, insulin resistance can be fully reversed — especially when caught early. The key is consistent lifestyle changes: a low-glycemic diet, regular physical activity, adequate sleep, and stress management. Some people have normalized their blood sugar markers within 3–6 months of committed lifestyle changes. However, if type 2 diabetes has already developed, management rather than full reversal may be the more realistic goal.
What foods should I avoid with insulin resistance?
The most important foods to limit are refined carbohydrates and added sugars: white bread, white rice, sugary drinks (including fruit juice), pastries, candy, and most ultra-processed snack foods. These cause rapid blood sugar spikes that force your pancreas to pump out more insulin, worsening the underlying resistance over time.
Is insulin resistance the same as diabetes?
No, but it is a major precursor. Insulin resistance is the condition where your cells don’t respond well to insulin — your blood sugar may still be normal because your pancreas is working overtime. Prediabetes develops when blood sugar begins to rise consistently. Type 2 diabetes is diagnosed when blood sugar levels exceed a specific threshold, and the pancreas can no longer compensate. Think of insulin resistance as the first warning sign, prediabetes as the second, and type 2 diabetes as the third stage.
How long does it take to reverse insulin resistance?
With consistent effort, many people begin to see improvements in insulin sensitivity within 2–4 weeks of starting regular exercise and dietary changes. Significant reversal of insulin resistance markers typically takes 3–6 months. Complete normalization can take 6–12 months or longer, depending on severity and individual factors. The earlier you start, the faster the results.
Can thin people have insulin resistance?
Yes, absolutely. While obesity significantly increases the risk, normal-weight individuals can also develop insulin resistance — sometimes called “lean insulin resistance” or TOFI (thin outside, fat inside). These individuals have normal body weight but carry excess visceral fat around their organs, which drives insulin resistance just as powerfully as visible obesity. Regular blood tests are the only way to know for sure.
What is the best exercise for insulin resistance?
Both aerobic exercise and strength training are highly effective, and combining them works best. Walking, cycling, and swimming improve cardiovascular insulin sensitivity. Resistance training (lifting weights, bodyweight exercises) builds muscle mass, which is the body’s most important glucose-absorbing tissue. Even 30-minute daily walks combined with 2–3 sessions of strength training per week can dramatically improve insulin sensitivity within weeks.
Medical Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider for personalized guidance.

David Miller: I am a health and wellness writer focused on diabetes awareness, blood sugar control, and healthy living. I creates clear, practical content to help readers make better everyday health choices. I write evidence-based articles about diabetes, diet, and healthy living. My goal is to simplify complex health topics using trusted sources like WHO and medical journals.